Making Big Data Work: The Promise and Potential to Transform Healthcare
To realize the benefits of big data in healthcare, technical, regulatory, and financial hurdles must be overcome.
December 10, 2014

Bill Betten
Today we hear a lot about big data and how it will revolutionize our lives in variety of ways. In healthcare, big data offers breakthrough possibilities from increased efficiencies and better outcomes to lower costs and more personalized care. But as connected applications provide us with more data than ever before, many organizations are struggling with what to do with that data to take full advantage of its potential.
This article explores some common pitfalls of big data in the medical industry and discusses strategies to leverage this data to affect change and improve healthcare.
Hear Bill Betten's talk, "Wellness-Integrated Medical Technology for Widespread Adoption," at BIOMEDevice Boston on April 14, 2016. |
The amount of information being generated in the healthcare industry continues to grow, driven by recordkeeping, compliance and regulatory requirements, and patient care. It is estimated that approximately 150 exabytes of data are contained within the healthcare system today. Historically, much of this was kept in paper form, but now it is being digitized and stored. As indicated in Figure 1, today islands of information exist within the healthcare environment. Each of these repositories has the potential to help improve healthcare if they can be tied together. Benefits to be gained by this integration include addressing healthcare personnel shortfalls, improvements in operational efficiency, reduction in costs, improved risk reduction and compliance, enhanced quality of care through improved data accuracy and utilization of decision support systems, and the potential to generate insights from big data analytics.
Figure 1: Information repositories in a clinical environment
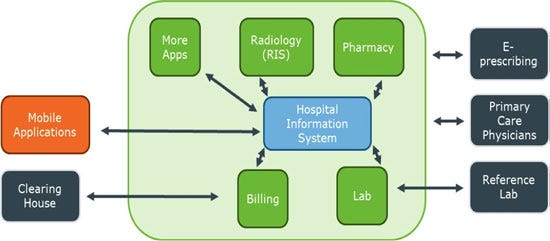
But there are technical, regulatory, and financial barriers holding back the integration of these various information sources. The technical barriers are typically related to standards and connectivity of the varied sources of information. The regulatory barriers are primarily security of information, privacy, and safety from hacking, rather than the clinical efficacy challenges typically associated with the medical device space. Finally, the financial barrier is associated with the perceived economic benefit of providing this connectivity to disparate stakeholders. These barriers have kept the growth and integration of data in the healthcare industry behind those of other industries (Figure 2).
Figure 2
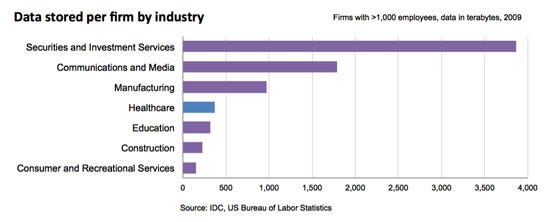
These barriers are rapidly being addressed, but other challenges are also emerging. One is the variation in the volume of information due to the variety of sources and their data attributes. Medical imaging files, for example, can consume a large amount of storage space, while text files and reports are relatively limited.
A second constraint is the pace at which the information is gathered. Continuous monitoring of a client can result in a challenging set of tradeoffs associated with how much data to collect and how often to collect it. The asynchronous nature of the various sources as well as the timeliness associated with the information can have a large impact on the architecture of an overall solution.
A third consideration is the variety of different formats of information to be gathered. The various information sources are not necessarily linked in a fashion to permit easy integration. An additional challenge in the information integration scenario is the growing influence of the consumer space, with many new devices generating information that, while of questionable medical value today, may prove valuable in the future, either as the devices are enhanced to provide medically relevant information or as it is viewed in the context of the rest of the data.
To overcome these challenges, it is important that standard interfaces be defined and utilized. This was successfully done in the 1990s with the development of the Digital Imaging and Communications in Medicine (DICOM) standard, which enabled the successful implementation of picture archive communication systems (PACS) for the medical imaging market. Prior to this, various manufacturers’ systems operated as islands of information, with that knowledge typically captured on a piece of high quality film. With the advent of standards, and as transmission and display technologies improved, the ability to send images across the world to wherever they are needed has become routine.
The financial hurdle is perhaps more complex as we seek to connect medical devices that have a variety of paradigms, ranging from expensive in-hospital monitoring to remote monitoring devices intended for monitoring the chronically ill or recently released patients. In fact, financial penalties associated with readmission of patients have provided one of the strongest drivers to establish a monitoring program postrelease.
As these hurdles are addressed and big data comes together in the healthcare space, we may finally see the benefits of sensor fusion, providing new ways of combining information that may improve healthcare outcomes. Today’s healthcare focuses on treatment of sickness. As we integrate additional information from the proliferation of consumer devices that are starting to become available, perhaps we can focus on treatment of wellness, with an emphasis on holistically managing the health of an individual. The real challenge is turning big data into real information and ultimately into actionable behavior change that results in improved outcomes (and perhaps no outcomes due to prevention). Perhaps then we can see some of the more than $300 billion in savings per year in the United States healthcare system could realize through big data analytics.
Bill Betten is vice president of business Solutions at Logic PD. He also serves on MD+DI’s editorial advisory board.
[main image courtesy of STUART MILES/FREEDIGITALPHOTOS.NET]
You May Also Like


