Pandemic Recovery for Hospitals Necessitates New Shared-Risk Model
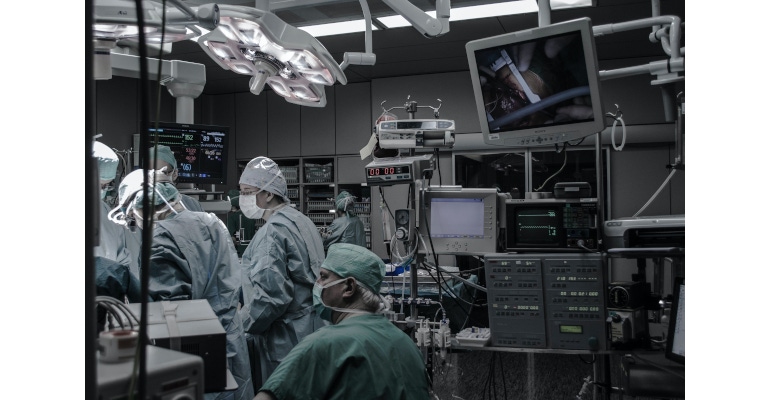
Operational costs could replace capital costs, which could give more surgeons access to advanced surgical equipment such as surgical robotics.
October 15, 2021
The financial impact of the COVID-19 pandemic on hospitals has reached existential levels, driving some fully out of business and significantly impairing the viability of others. The American Hospital Association estimated that hospital and health system losses amounted to at least $323.1 billion at the end of 2020. The fiscal impact is still rising. Recovery for any hospital will likely not be a return to business as usual. There are lessons to be learned and necessary shifts to ensure the long-term health of each hospital.
One shift will be toward a new model for outfitting operating rooms with surgical equipment. The pre-pandemic model involved mainly large capital purchases or expensive leasing through a vendor or third-party. It placed the burden squarely on hospitals and forced various decisions and practices. A new model is taking root that not only eases financial burdens for what had been capital equipment but also shares the risk associated with it. It creates a deeper partnering between vendors of state-of-the-art equipment and hospitals to ensure higher levels of utilization and success.
The shared risk model has existed at least since 1997, when an article appeared in Healthcare Financial Management, the journal of the Healthcare Financial Management Association, detailing a procurement model in place at The Medical Center at the University of California, San Francisco (UCSF). In this case, UCSF developed a way to manage the cost of pumps for infusion therapy. The arrangement, with a particular vendor, set a fixed payment schedule for more than 700 pumps, maintenance, full warranties and applicable upgrades, enabling UCSF to serve more patients and engage in cutting-edge treatments. It was devised to manage costs, maintain an adequate supply of infusion pumps to meet typical demands, and ensure a proper level of equipment utilization.
A new kind of shared risk model is emerging that is similar in large part to the Software-as-a-Service model (SaaS) that is now the prevalent way to acquire software applications today. Few enterprises or organizations would opt to purchase a perpetual license to software for accounting, sales process, marketing operations, or HR. The norm is a pay-as-you-go model based on number of seats, availability of options, and elapsed time. With this sort of approach, hospitals can pay for a piece of surgical equipment—surgical robots, for instance—on a per-use basis. Capital costs move completely over to operational costs, so to speak.
Utilization models can shift from a place where there is a strong incentive to recover sunk capital costs to one that is mostly free from financial pressures and mostly geared to medical and treatment criteria. Eliminating pressures for CAPEX to be recouped, surgical robots become no longer a “solution in search of a problem.” Costs for the robots would only be incurred with each use, enabling more appropriate pricing models and treatment plans best suited for each case.
The manufacturers would bear most of the risk and capital cost burden, but they would receive an ongoing revenue stream. Maintenance, support, and training could be built into the per-usage charges or offered for a specified span of time, such as per-month or per-year. Rolling up all costs into complete per-usage pricing is the most probable case.
In all likelihood, manufacturers would gain significantly more customers, since a much larger number of facilities could now afford their solutions. Advanced surgical equipment would no longer be limited to the largest, best-funded hospitals or those that have secured special grants to fund such acquisitions. Producing a larger number of, say, surgical robots and having far more usage would likely spark greater innovation by the manufacturers for improvements and additional features based on a broader, and perhaps deeper, usage. More surgeons would gain access to and experience from the equipment, improving techniques for using it and contributing toward best practices. This knowledge and experience could drive demand for greater numbers of this equipment.
Versatility may be another benefit from such a new model of making surgical equipment available. Surgeons may find new ways to utilize the solutions, and vendors may create equipment that is more flexible and feature-rich. Such a dynamic lends away from one-trick-pony solutions to ones that can be used more broadly or deeply.
Hospitals will be examining the financial impact of everything. Besides new procurement models that shift away from capital outlays, they will be interested in things that reduce operational costs. They will want to expand elective offerings, according to demand and opportunity, particularly in keeping patients local rather than sending them off to a larger facility at some distance away. Hospitals will be attracted to equipment that can lower the cost of procedures, lessen the number of medical professionals involved, and be more “resistant” to the potential interruptions caused by pandemic surges or new outbreaks. New breeds of surgical robots could potentially offer these benefits, if they can be made affordable.
The pandemic did not create these new dynamics out of the blue. These are considerations, and even desires, that have existed for some time. The pandemic has become a powerful catalyst to demand or require change. Many hospitals are in survival mode, and, for them, many things must change. Risk and financial burden need to shift. The result can bring substantial benefit to all.
About the Author(s)
You May Also Like



