These Electrodes Melt in Your Brain, Not in Your Hand
May 10, 2016
The devices may have implications for epilepsy, Parkinson's disease, depression, chronic pain, and peripheral nervous system conditions, and may improve postoperative monitoring.
Nancy Crotti
Researchers at the University of Pennsylvania have invented an implantable electrode that melts in the brain to minimize tissue injury.
Compared with current postoperative monitoring practices, the electrode may be useful following vascular, cardiac, and orthopedic procedures, according to the study, published in Nature Materials.
"Dissolvable silicon electronics offer an unprecedented opportunity to implant advanced monitoring systems that eliminate the risks, cost, and discomfort associated with surgery to extract current devices used for postoperative monitoring," said senior co-author Brian Litt, MD, a professor of neurology, neurosurgery, and bioengineering, in a university news release. "This study tested the usefulness of temporary, dissolvable monitoring systems capable of providing continuous streams of data for guiding medical care over predetermined periods of time --from days to months--before dissolving."
Litt led the study with long-time collaborator John A. Rogers, PhD, a material scientist from the University of Illinois at Urbana-Champaign who is a flexible electronics pioneer.
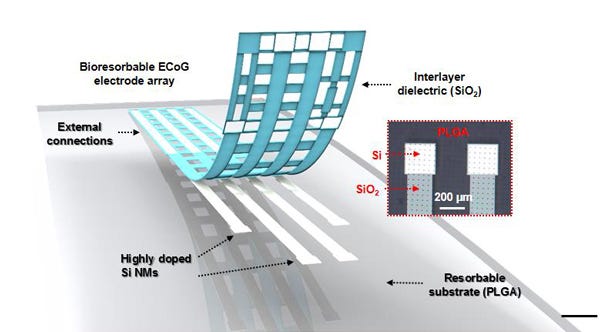
The device is made of layers of silicon and molybdenum that can measure physiological characteristics. It dissolves at a known rate, determined by its thickness. At present, postoperative monitoring is based on clinical examination or interventional radiology, which is invasive, expensive, and impractical for continuous monitoring over days to months.
The researchers used it to record brain waves in rats under anesthesia, as well as voltage fluctuations between neurons (EEGs), and induced epileptic spikes in intact live tissue. Separately, they measured the sensing capabilities of rat whiskers in high resolution, using a complex, multiplexed array made from the same materials. Devices placed at the outer layer of brain cortex tissue and the inner space between the scalp and skull recorded the electrophysiological signals.
The device measures the type of neurophysiologic features commonly used in diagnosing and treating such disorders as epilepsy, Parkinson's disease, depression, chronic pain, and conditions of the peripheral nervous system, according to Litt.
"These measurements are critically important for mapping and monitoring brain function during and in preparation for neurosurgery, for assisting in device placement, such as for Parkinson's disease, and for guiding surgical procedures on complex, interconnected nerve structures," he said.
Other applications include post-operative monitoring and recording of physiological characteristic after minimally invasive placement of vascular, cardiac, orthopedic, neural or other devices. It could mark an improvement over interventional radiology, which the researchers characterized as invasive, expensive, and impractical for continuous postop monitoring over days to months.
Researchers in China reported separately on the technology in Nature Materials, saying it "offers general applicability in neural interfaces, with additional potential utility in treatment of disorders where transient monitoring and modulation of physiologic function, implant integrity and tissue recovery or regeneration are required." A report on the Chinese researchers' work and related technology appears in the Kurzweil Accelerating Intelligence.
The electrode is just the latest in the wave of bioabsorbable devices being tested for use in humans.
It performed as well or better relative to conventional electrodes used in the clinic, in terms of tissue reactivity, cellular, and immune staining after the end of comparative studies, the university reported.
The team sees numerous uses for the implant, such as monitoring postoperative seizures and recovery of brain function after surgery, aneurysm coiling, stent placement, embolization, and endoscopic operations. The device could also monitor structures that are exposed during surgery but are too delicate to remove.
Partially funded by DARPA, the research will continue to develop more complex devices that include flow, pressure, and other measurement capabilities.
Check out more medtech-related electronics advances>>
Learn more about cutting-edge medical devices at MD&M East, June 14-15, 2016 in New York City. |
Nancy Crotti is a contributor to Qmed and MPMN.
Like what you're reading? Subscribe to our daily e-newsletter.
About the Author(s)
You May Also Like



.png?width=300&auto=webp&quality=80&disable=upscale)
