Matters of the Heart: AEDs Go Public
Medical Device & Diagnostic Industry MagazineMDDI Article IndexOriginally Published March 2001
March 1, 2001
Medical Device & Diagnostic Industry Magazine
MDDI Article Index
Originally Published March 2001
Gregg NighswongerMore than one million deaths each year in the United States are attributed to cardiovascular disease. Over one fourth of these deaths are caused by sudden cardiac arrest (SCA)—particularly as a result of ventricular tachyarrhythmias. The overall survival rate for SCA victims ranges from 1% out of hospital to 15% in hospital, and the most effective treatment has been found to be immediate defibrillation. In 1996, the American Heart Association (AHA) announced that prompt defibrillation is the single most important therapy for the treatment of SCA. The AHA estimates that administering timely treatment could save as many as 100,000 SCA victims per year.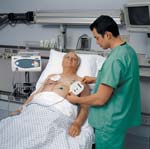 Legislation has increased public access to AEDs, once used only by trained hospital and emergency personnel.
Legislation has increased public access to AEDs, once used only by trained hospital and emergency personnel.
Cardiopulmonary resuscitation (CPR) is also used to treat SCA, and the administration of CPR by bystanders has been associated with slight reductions in the number of deaths resulting from cardiac arrest. Even with the use of CPR, however, only 5% of individuals experiencing cardiac arrest survive, while prompt treatment with external defibrillators has been shown to improve survival rates significantly. Now, advances in portable defibrillator technology and recent legislative activity may make public access to defibrillation more common, increasing survival rates for SCA.
A MANDATE FOR PUBLIC ACCESS
The Cardiac Arrest Survival Act (CASA) and the Rural Access to Emergency Devices Act, which were signed into law on November 13, 2000, were aimed at increasing public access to automated external defibrillators (AEDs). Applauded by the AHA, the new legislation requires the Secretary of Health and Human Services to develop recommendations and specify guidelines for AED placement and use in federal buildings and augments existing state "Good Samaritan" laws by ensuring federal liability protection for purchasers and users of AEDs. CASA was cosponsored by more than 130 legislators and was backed by a coalition of more than 30 healthcare organizations.
Senator Bill Frist, MD, of Tennessee, a heart surgeon and leading cosponsor of CASA, describes it as "a fundamental first step to ensure that cardiac arrest is not a death sentence. Widespread placement of AEDs in federal buildings will save lives, but communities still need to do more. We need to make portable, easy-to-use external defibrillators as readily available as first-aid supplies and fire extinguishers in all major public gathering places." Increased AED availability is being offered as a new standard of care for emergency cardiac situations in public gathering places—airports, shopping malls, stadiums, convention centers, schools, and office buildings.
INSIDE AN AED
AEDs are basically external defibrillators that incorporate a system for analyzing cardiac rhythm. Available devices range from shock-advisory units to semi- and fully automatic models. Adhesive pads and cables are used to attach the AED to the patient, record cardiac rhythm, and deliver the necessary electric impulse, or shock.
While shock-advisory and semiautomatic systems require the operator to take additional steps in controlling shock delivery, fully automated systems only require the operator to attach the pads and initiate the system. The device then initiates its rhythm analysis cycle and, if ventricular fibrillation or rapid ventricular tachycardia is detected, charges its capacitors and requests delivery of a shock—repeating the cycle as needed.
Human factors, efficient microprocessing, and effective use of internal memory have been vital issues in AED design and development. Most devices incorporate voice prompts to guide users in the defibrillation process. Labeling of the AED electrode has been designed to ensure correct placement on the patient. The result has been the availability of AEDs that can be operated with virtually no prior training.
INCREASED PUBLIC ACCESS
More than 40,000 AEDs have been deployed in police cars, commercial aircraft and airports, hotels and casinos, sports arenas, high schools, manufacturing plants, and various other public places. In hearings over the past two years, legislators heard dramatic testimony from cardiac arrest survivors and emergency service directors, and viewed a casino surveillance video that showed the rescue of a victim using a Medtronic Physio-Control Lifepak 500 AED.
 Human factors has been an essential element in the development of AEDs for public access.
Human factors has been an essential element in the development of AEDs for public access.
Susan Martenson, RNCEN, vice president of Jane Phillips Medical Center (Bartlesville, OK) and a CPR instructor, states, "Technology has advanced to the point where real people can make a significant difference." Using funds received for participation in clinical research, Martenson and Patrick Tinker, MD, a cardiologist, have led Bartlesville's Project Heart-Save, which has trained more than 300 residents in the city of 35,000 to use AEDs. The program also has placed about 20 of the devices in various public buildings, such as the hospital's wellness center, medical office clusters, the county courthouse, a country club, a YMCA, the senior nutrition center, a technical college, and a shopping mall.
The key to increasing public access to life-saving AEDs has been to simplify operation of the devices. Results from a number of studies appear to support the idea that device effectiveness can indeed be maintained while designing for ease of use.
In a study conducted by Terence D. Valenzuela, MD, of the University of Arizona Sarver Heart Center (Tucson, AZ), casino security officers trained in AED use observed approximately 150 SCA cases and used AEDs on 105 of these individuals. More than half of these individuals survived to hospital discharge, according to Valenzuela. He adds that nearly 75% of those receiving AED treatment within three minutes of the onset of SCA survived, compared with only half of those defibrillated after more than three minutes.
Success in developing easy-to-operate AEDs, and in initial public access programs, is prompting availability of the devices in a broader range of public areas. In January, for example, the Building Owners and Managers Association (BOMA) International began a six-month research effort to assess the benefits and liabilities of placing AEDs in privately owned commercial buildings.
BOMA's action is partially predicated on the group's intention to push for increased Good Samaritan protection for individuals using AED equipment. Says Richard D. Baier, BOMA president, "Without the specter of a lawsuit should the equipment fail, we believe more building personnel would be willing to get the training, have the devices on-site, and jump in and try to save someone in a cardiac emergency."
SIMPLE ENOUGH FOR A CHILD TO USE
A study conducted in Seattle found that sixth-grade school children with moderate training can learn to use AEDs to save the lives of cardiac arrest victims almost as quickly and efficiently as professional emergency medical personnel, according to a recent report in an AHA journal.
Although previous studies have shown that trained nonprofessionals had little difficulty using AEDs on real patients, this was the first AED study involving children. "Now we know that AEDs are literally easy enough for a child to use," says Gust H. Bardy, MD, of the University of Washington Medical School (Seattle). "There is a persistent idea that many hours of special training are required to operate an AED," Bardy explains. "But the fact is, these machines are incredibly easy to use."
For the study, a group of researchers from the University of Washington recruited 15 sixth-grade pupils from a private school who had received parental permission to participate. The students were given brief instructions on how to remove the packaging from the electrode pads of the AED. They were also instructed on how and where to properly place the pads on a mannequin's chest so that the electrical shock to defibrillate the heart would be given safely and correctly.
The children were not allowed to ask questions during the subsequent test, and researchers provided no other guidance. Their performance times were compared with those of 22 trained emergency medical technicians and paramedics who also had no previous experience with this specific type of defibrillator but had been trained in defibrillation and cardiac arrest rehabilitation.
Says Bardy, "It took the sixth-graders an average of 90 seconds to complete the defibrillation compared to 67 seconds on average for the EMTs/paramedics." He adds that all of the study participants correctly placed the electrode pads, and remained clear of the "patient" during shock delivery.
After completing the test, 14 of the 15 sixth-graders said they felt confident that they could teach someone else how to correctly use the AED. All of the students said they believed they could use the AED on a family member should the need arise.
SAFEGUARDING AIRLINE PASSENGERS
A significant portion of public experience with AEDs has been aboard aircraft. For example, during a study conducted in association with American Airlines, researchers at the University of Texas Southwestern Medical Center (Dallas) found that AEDs used by airline flight crews were useful in saving the lives of sudden cardiac arrest victims aboard aircraft and for use in monitoring patients. AEDs were initially available only during over-water flights and were then added to other American Airline flights. Flight attendants received four hours of classroom and workshop instruction followed annually by a refresher course and examination.
The study found that 40% of those who were treated with an AED survived during the two-year American Airlines study. According to Richard Page, MD, director of clinical cardiac electrophysiology at UT Southwestern, a means of treating sudden cardiac arrest victims aboard aircraft had been needed for years. "This is an isolated environment. If something goes wrong, there's not a backup immediately available. After 10 minutes, the victim's chance of survival is extremely small. Even if an aircraft is close to landing, that may take at least 20 minutes. If you get to someone fast, you have a high chance of resuscitation."
During the UT Southwestern study, which ran from June 1997 to July 1999, an AED was used on 200 patients as a monitor and to administer shock. Page explains that "the victim must have ventricular fibrillation to require a shock. Not everyone who loses consciousness needs a shock. They may be in normal rhythm and have passed out, or they may already be dead and not have a rhythm or have a flatline rhythm. In those cases, no shock should be administered."
Electrical shock was administered to 15 people experiencing ventricular fibrillation. Four of the 15 patients who received shocks had cardiac arrest in the airport terminal. None of these patients survived. The remaining patients receiving shocks had cardiac arrest aboard the aircraft. Of those 11 patients, six survived. After being removed from the aircraft, the six patients were transferred to a hospital and later discharged at their full functional status.
The rate of survival after defibrillation was 40%. Says Page, "The percentage compares favorably with the rate of survival to discharge among patients who received a defibrillator shock in a setting other than an airliner." He adds that, "The device was also safe when used as a monitor; in no case was an inappropriate shock recommended or delivered. Our experience on the airlines showed that the devices are safe even when used outside of label indications, as there were no ill effects when the device was placed in the absence of loss of consciousness (101 of 200 total)."
The researchers analyzed data collected from electrocardiograms (ECGs) used to measure electrical activity in the heart. Using these data, cardiologists were capable of evaluating the function and safety of the device. (ECG data were available for analysis in all but 15 cases.)
Page foresees greater public use of AEDs in the near future. "I anticipate that AEDs will be used more and more by less-trained persons. This is appropriate, given the safety and simplicity of these devices. It has been shown that sixth-graders without training can operate the AED in just 90 seconds. As awareness is increased, and the AEDs are placed universally, I would see any crowd as having persons qualified to use the device. Furthermore, minimal training should be adequate." He adds, "The devices are becoming quite mature. What remains to be established is the infrastructure to support the devices and adequate public awareness and training. The device of the future might have automatic EMS calling and further interactive capabilities."
Strategically placing AEDs one minute apart and making them easy to spot has helped prevent sudden cardiac deaths at Chicago's heavily trafficked O'Hare and Midway airports, according to a study presented at the AHA Scientific Sessions 2000 meeting. The City of Chicago Airport System's HeartSave Program placed 49 AEDs on walls throughout O'Hare and Midway airports in June 1999. Two more AEDs were placed in parking facilities. Approximately 80 million passengers each year travel through O'Hare and 20 million move through Midway. The devices were mounted in plain view. With easy-to-use audio and visual prompts, the devices helped reduce critical response times to emergency care.
In the first 10 months of operation, 14 sudden cardiac arrests occurred; 12 of the 14 victims were in ventricular fibrillation and 9 of the victims were revived with an AED. Victims who were revived using the AEDs were found to have sustained no neurological damage. In nine of the incidents, airport travelers successfully operated the devices, rather than on-site staff formally trained as part of the airport's HeartSave Program. In places without rapid response to instances of cardiac arrest, survival has averaged 4%.
"Easy access and high visibility may be ingredients for success," says the study's lead author, Paula J. Willoughby, DO, emergency medical services advisor for the Chicago Fire Department. "The real issue right now for these devices is where to put them."
"When these devices were first introduced, there was a lot of trepidation about where to put them and whether people would get shocked right and left if the lay public used them," Willoughby says. "Our data suggest that these devices can be simple to use and that the public can use them properly when given simple instructions. Putting portable defibrillators in commercial aircraft and at airports would save both lives and money for the airlines."
INCREASING LAYPERSON USE
According to Kenneth F. Olson, vice-president of R&D at Survivalink Corp. (Minnetonka, MN), "Survivalink is a major contributor to the Public Access Defibrillation (PAD) Study being coordinated by the University of Washington. The study is also supported by the National Institutes of Health, the American Heart Association, and other manufacturers. It is the first study to actually attempt to measure the effectiveness of AEDs in the hands of lay responders. It has taken us four years to get this study under way, and it is sure to be a landmark study." Olson states that there are several key issues to be addressed in providing public access to AEDs.
Ease of Use. "The devices have to be very simple to use. This involves driving the number of user-critical steps to an absolute minimum," says Olson. A user-critical step is an operation that must be performed to successfully complete a rescue attempt. Olson explains, "With lay responders a certain number of individuals will fail to complete each operation, no matter how elementary the operation. Even more importantly, the lay rescuer will not have the cognitive ability to recover from a failed operation. They will typically just give up. This is due to several factors, not the least of which is that they are already operating in an uncomfortable environment—the application of medicine to an unconscious person. It is vital for us to remember these individuals are not medical people."
"To help counteract this, we minimize the number of steps," Olson continues. "But we also utilize voice prompting to help talk users through the procedure. The voice prompts are currently targeted for a minimally trained individual. For a true layperson, they may need to be expanded, yet this also has drawbacks. Expanding the voice prompts can slow down the entire rescue attempt."
Low Cost. The list prices for AEDs are currently in the $3000–$4000 range. Olson suggests that this range needs to be lowered if there is going to be a broad penetration into truly lay markets.
Low Maintenance. Maintenance of defibrillators is a major concern, according to Olson. "Only a few short years ago, the recommended maintenance was a 20-minute procedure that was conducted daily. With the development of our first AED, the Vivalink, we incorporated that testing into the device." He adds that "this reduced maintenance to recharging the battery monthly, and looking at a status indicator daily. The self-tests have gotten even more sophisticated, and the devices now can very much take care of themselves."
Olson explains that one critical component of available AEDs is the electrodes. "Electrodes are water based and they dry out with time. They all contain an expiration date ranging from one to two years. This is a very real problem, because old electrodes may be unusable for conducting a rescue, and they need to be replaced prior to expiring." The electrodes may also be missing from the AED. According to Olson, 40% of reports made to FDA about an inability to use a defibrillator at a rescue involve failed or missing electrodes.
Analysis Algorithms. The algorithms used by the AED to determine when it is appropriate to deliver a shock are a vital part of the system. Says Olson, "They are all designed to withhold therapy in the case of an inconclusive ECG. This means they have very high specificity. They are also good at determining when a shock is necessary, which is sensitivity. But the current algorithms are all designed with the presumption that the device is being used properly, i.e., on someone who is unconscious, not breathing, with no pulse." Effective use by lay responders requires the algorithms to be robust enough to retain adequate specificity, Olson states, "even in the event the device is misused. To obtain this may mean reducing sensitivity in some cases."
Survivalink is the developer of the FirstSave AED, which uses one-button operation and provides preconnected, interchangeable electrodes. According to the company, the device is also the first AED to incorporate an escalating, variable-energy biphasic waveform, which was found to be 100% effective in clinical trials.
The unit also incoporates certain human factors elements in its design to simplify use by untrained individuals. For example, the use of preconnected electrodes that are stored inside the device eliminates the need to plug in electrodes during the rescue. The company explains that this eliminates a user-critical step.
In addition, the electrodes are nonpolarized and are specifically labeled for interchangeable use. Either electrode can be placed on the upper right or lower left of the patient's chest.
The device also incorporates a number of other design concepts that were previouly used only in implantable defibrillators. The company explains that its proprietary Star biphasic technology "introduced escalating biphasic energy and developed the concept of customized, variable energy."
Conventional biphasic waveforms deliver a fixed energy level regardless of patient needs. The Star biphasic system, however, varies the level of energy delivered to each patient based on the charge balancing principle. "This principle states that once a defibrillation charge is given, excess or residual charge on the heart's cells must be neutralized to prevent refibrillation. Star biphasic is the only defibrillation waveform to successfully address this principle," according to the company.
THE AED MARKET
According to a market analysis conducted by Frost & Sullivan (Sunnyvale, CA), external defibrillator suppliers in the United States, Europe, and Japan accumulated revenues totaling more than $392 million in 1999. These numbers are expected to grow to more than $1 billion by 2006, according to the company.
The Frost & Sullivan report, U.S., European, and Japanese External Defibrillator Markets, indicates that "there is not yet a market for public access defibrillators (PADs) in Japan. However, the U.S. and European markets combined for revenues of nearly $67 million in 2000, with an expected compound annual growth rate of more than 35% through 2006." The firm suggests that manufacturers producing low-cost systems that are easy to use are the ones most likely to profit from this projected growth.
"The PAD market is in its very early stages of development, with the U.S. market being more developed than the European market," says Frost & Sullivan market analyst Harini Raj. "As for Japan, in the earliest case, [growth] could take three years, and at the latest, it could take as long as 8–10 years."
PROVIDING A NEW STANDARD OF CARDIAC CARE FOR HOSPITALS
The technology incorporated in the generation of AEDs that are making public access to defibrillation possible is also reflected in systems being used in hospital settings. Such systems provide advantages in monitoring critical-care patients, and can provide more rapid treatment by defibrillation when necessary.
For example, a new noninvasive defibrillation technology offers a unique alternative for monitoring and treating patients at risk of sudden cardiac arrest in the hospital setting. Developed by Cardiac Science Inc. (Irvine, CA), the Powerheart external cardioverter defibrillator-monitor (ECD) is a fully automatic device that received FDA special 510(k) clearance in January.
The company indicates that FDA has allowed for a broad intended use. The device is approved to detect and to provide automatic treatment for ventricular tachyarrhythmias of in-hospital patients who are considered to be at risk of sudden cardiac arrest.
The device is attached externally to a patient's chest via disposable electrodes in advance of any type of life-threatening situation. It continuously monitors the patient, instantly detects the onset of a life-threatening tachyarrhythmia, and, when appropriate, delivers defibrillation shocks within seconds and without the aid of hospital staff to reestablish the heart's normal rhythm.
The ECD technology has the same life-saving potential for hospital patients at risk of sudden cardiac arrest as the implantable cardioverter defibrillator (ICD) has had for out-of-hospital cardiac patients at permanent risk. An ICD is a miniaturized defibrillator implanted inside a person's chest and attached directly to the heart via electrodes. ICDs have been proven to save lives. The ECD is most simply described as the external embodiment of an ICD, according to Cardiac Science.
Clinical data compiled over three years from 155 patients at four nationally recognized medical centers validated the safety and efficacy of the new device. The ECD identified life-threatening shockable episodes with 100% sensitivity and demonstrated a specificity of 99.4% (not allowing nonshockable rhythms to be shocked).
The device's average response time to the first shock was only 21 seconds. First shock efficacy was 96.2% (converting a patient back to normal rhythm with one shock) with energy levels as low as 50 J (external defibrillators deliver energy up to 360 J).
Because response time to first defibrillation is critical, the new device provides significant patient benefits, the company claims. Similar to an ICD, it recognizes and quickly converts a life-threatening abnormal rhythm prior to the heart quivering. This allows for lower-energy shock levels, sparing the heart muscle damage, and prevents a loss of oxygen to the brain, eliminating potential neurological damage and a diminished quality of life. Overall debilitation may be lessened, recovery periods shortened, and hospital stays reduced.
Cardiac Science sponsored a symposium for cardiologists attending the 73rd Annual AHA Scientific Sessions to discuss ways to improve the 15% survival rate for patients who suffer cardiac arrest while in the hospital.
The symposium panelists included Ted Borek Jr., AHA vice president of emergency cardiac care programs, and Vinay M. Nadkarni, MD, chairperson of the AHA emergency cardiovascular care committee. The two men were responsible for developing the recently published revised guidelines that call for delivery of a defibrillation shock within three minutes after the onset of a hospital cardiac arrest.
"Today, there are significant delays in responding to patients in cardiac arrest in hospitals. These delays result in average response times of five to seven minutes," said panelist John P. Rudzinski, MD, vice chairman, department of emergency medicine, at Rockford Health System (Rockford, IL). "Delayed defibrillation can result in patient death, brain damage, or a diminished quality of life. For each minute that passes, a patient's chance of survival declines 10%. Defibrillation within seconds may reduce patient complications, shorten hospital stays, and reduce costs."
Panelist Thomas A. Mattioni, MD, director of electrophysiology at the Arizona Heart Institute and Hospital (Phoenix), added, "Powerheart can be invaluable in helping hospitals comply with the new AHA guidelines. It is as if a cardiac team is standing by the patient bed 24 hours a day, 7 days a week." He went on to report that the device has already saved patient lives, including several at the Arizona Heart Hospital.
CONCLUSION
With a legislative mandate, increasing public awareness, and the availability of effective new technologies, AEDs are saving the lives of more and more SCA victims. Current AEDs are literally simple enough for a child to use. A significant issue to be resolved, however, will be extending and possibly revitalizing Good Samaritan laws to safeguard those individuals who may be called upon to use an AED in an emergency situation.
Gregg Nighswonger is executive editor of MD&DI.
To the MDDI March 2001 table of contents | To the MDDI home page Copyright ©2001 Medical Device & Diagnostic Industry
About the Author(s)
You May Also Like

.png?width=300&auto=webp&quality=80&disable=upscale)
