Behind the FDA Submission: How J&J Won a Key Approval in AF Ablation
A behind-the-scenes look at how Johnson & Johnson approached a key regulatory submission involving several of its catheter ablation devices.
August 22, 2023
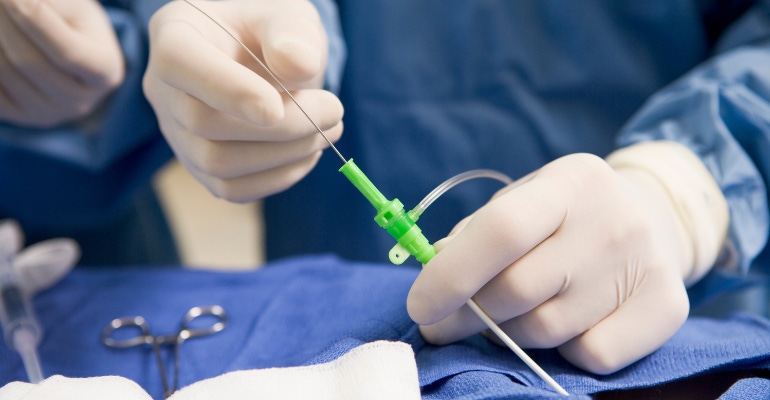
Biosense Webster, part of Johnson & Johnson MedTech, recently scored FDA approval covering several products in its cardiac ablation portfolio for use in for use in a workflow without fluoroscopy. The secret sauce behind the submission: real-world evidence.
Fluoroscopy is a type of medical imaging that shows a continuous x-ray image on a monitor and is used in a variety of examinations and procedures to diagnose or treat patients. Reducing reliance on fluoroscopy lowers radiation exposure for patients and gives clinicians a much-needed break from wearing heavy lead aprons to protect themselves from radiation exposure.
The products that can now be used in a zero-fluoroscopy workflow include: Thermocool SmartTouch SF catheter, Thermocool SmartTouch catheter, Carto Vizigo bi-directional guiding sheath, Pentaray nav eco high density mapping catheter, Decanav mapping catheters, and the Webster CS catheter. The updated workflow indicates that direct imaging guidance, such as ultrasound, may be used as an alternative to fluoroscopy.
The company received the label change based on an observational, prospective, multicenter registry that assesses real-world catheter ablation clinical outcomes, including procedural efficiency, safety, and long-term effectiveness in a broad group of patient populations with novel radiofrequency technologies in paroxysmal atrial fibrillation (AF) patients. The REAL AF registry is a real-world evidence registry in the electrophysiology field, led by physicians and supported by Biosense Webster since 2019.
To learn more about the secret sauce, so to speak, behind this FDA approval, MD+DI interviewed Anthony "Tony" Hong, VP of preclinical and clinical research and medical affairs for cardiovascular and specialty solutions at Johnson & Johnson.

MD+DI: Why is it important that these atrial fibrillation ablation products are approved for use in a workflow without fluoroscopy? In other words, what is the significance of that approval?
Hong: This the first and only FDA approval for a zero fluoro workflow with any ablation catheter, so I think this is a significant accomplishment for us in using real-world evidence to really demonstrate how products are being used in safe and effective ways. And the reason why I think this is significant – besides the fact that this is really the first approval based on real-world evidence – is really for the benefit of patients and physicians, and this is why we did it. ... Oftentimes if you think about physicians that are doing these cases day in and day out – and they may be doing multiple cases throughout the day – they're having to wear lead to protect themselves from the continuous x-ray, the fluoro. Not only does that have a significant health impact from potential long-term cancer risk, but also orthopedic (injury) from the lead. I've been in labs wearing lead and when you're standing around for six hours, seven hours you really feel it, and if you're doing this every day, it's a significant impact on the physicians that are doing the treatment. So, there's a there's a benefit to physicians knowing that there are products out there that they can do procedures without fluoro.
And secondly, it's also for the benefit of patients because when patients are undergoing these procedures while they're not exposed to the length that physicians are, they're still exposed to x-ray radiation, and so minimizing or eliminating that is a benefit to the patient who is undergoing the procedure. It kind of reminds me of when I go to the dentist's office and when they want to do an x-ray on your teeth, they put the lead on you and even though it's for literally a split second, you're still concerned about that x-ray. Well, when you're doing an ablation procedure that could last an hour, maybe more, and if the physician is using a lot of fluoro, that's also exposure for the patient.
MD+DI: You mentioned the use of real-world evidence, and I just wanted to circle back on that and ask you to elaborate on the importance of taking that evidence generation approach and using real world evidence to pursue a regulatory approval of this type.
Hong: Historically, end products in order to come to market are done under what's called an IDE (investigational device exemption), so we're running company sponsored IDE trials from a product approval perspective, but I often say that the hurdle for product approval is sometimes lower than the hurdle for product adoption. And so, we have to consider the evidence sharing needs for demonstrating the value and certainly supporting the claims of any product and when we run IDE trials and then subsequently do alternative channels of evidence using real-world evidence to corroborate that data, that data becomes even more powerful. So, I've often said if I'm running a 500 patient IDE and it shows great results it's fantastic, but if I can now do real-world evidence with even more patients and seeing how that product is actually being used in the public by the physicians in a real-world environment and that data corroborates the IDE it's very powerful. As we speak with the FDA, we are looking at how products are used beyond the IDE, how physicians are using these products in a real world setting and treating patients and showing how that can be done safely and effectively. This is why the FDA is also very interested in seeing more and more real-world evidence efforts which is also tied to how we were able to get the persistent indication for our SmartTouch catheter using real world evidence so there's a genuine interest among regulators and seeing how products are used in the real-world environment.
This is why we embarked on this, and I think this has been a tremendous partnership with the FDA and, we see this as an opportunity to continue to do more real-world evidence.
MD+DI: Aside from the obvious clinical benefits of having that real world evidence back up the IDE evidence, are there any potential benefits to the sponsor, the company that’s pursuing it, in terms of speed or cost?
Hong: From a speed perspective the data gathering, and data analysis will still take a bit of time because you have to make sure that the real-world data that you're gathering is in fact collected in the appropriate way. So oftentimes the notion that, “garbage in gives you garbage out,” is absolutely true and we have to make sure that the data collection among the sites that we’re working with has been very robust, and so that takes a little bit of time. And then of course everything is done prospectively from an analysis perspective and then once that's submitted the FDA's review time for real world evidence, at least in our experience, has been a little bit faster than the review for PMA's and so there could be a bit of a cost/time savings and from a cost perspective running prospective IDE can be quite expensive and real world evidence could have a benefit from a long term cost perspective of generating evidence for getting label changes.
MD+DI: From a technical or regulatory perspective, were there any other hurdles that needed to be overcome to win this FDA approval?
Hong: From a technical perspective I think it was just making sure that we have early alignment with the FDA … the early partnership with the FDA and the early communication and alignment I think is very important, but that's true with any regulatory body. As we work on real world evidence it's really important to align with the regulatory agency in proposing exactly what data we want to use, how we want to do the analysis, and aligning on what the endpoint parameters are. … Not an overwhelming challenge but it really required the cross functional teams within Biosense to make sure that we were fully aligned on what that finish line was going to be.
MD+DI: If you had to do this regulatory submission all over again is there anything you would do differently?
Hong: This one was, in my mind, a home run. I think it really demonstrated the cross functional and cross industry and FDA partnership. There were, in my mind, no major hiccups, so I'm not sure that I would change anything.
MD+DI: Is there anything I haven’t asked that you'd like to tell me about this regulatory approval?
Hong: …I think it really goes to show how we are continuing to push the envelope. I often talk about the importance of converging technology with technique – you can have great technology but if it's not being used in the appropriate way then it may not serve a benefit to patients. As we think about the evidence to support the technologies that we're building and how physicians are using them in the real world and how that leads to differentiated and potentially better outcomes for patients, that's really what we're continuing to push with our clinical science activities. It’s something that I continue to push my team to do more of.
About the Author(s)
You May Also Like



