Magnetic Sensors Carry Ultrasound to Greater Heights
Ultrasound is being used at the point of care—and not just for biopsies, thanks to technology advances such as magnetic sensors.
June 28, 2011
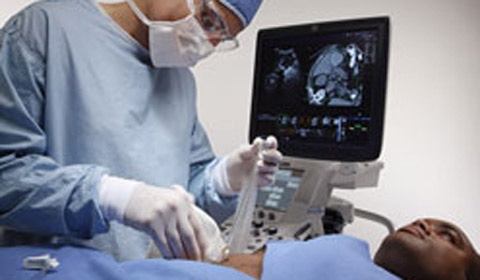
The roots of ultrasound run deep. An Italian scientist in the late 18th-century theorized that bats navigate using sound, giving rise to basic principles of ultrasound.
The transition to medical imaging came much later when, in the 1940s, a Naval Medical Research Institute physician demonstrated the detection of gallbladder stones using A-mode metal-flaw detectors and naval sonar. Medical ultrasound was born.
 Since that time, the modality has proven to be a significant diagnostic tool with numerous clinical uses—one that, unlike computed tomography (CT), does not expose patients and users to potentially harmful radiation. Still, historically both CT and magnetic resonance imaging have overshadowed it, at least in terms of public consciousness.
Since that time, the modality has proven to be a significant diagnostic tool with numerous clinical uses—one that, unlike computed tomography (CT), does not expose patients and users to potentially harmful radiation. Still, historically both CT and magnetic resonance imaging have overshadowed it, at least in terms of public consciousness.
That perception, however, is changing, due to several important advances: the tool’s emergence from 2-D to a volumetric imaging modality, the steady evolution of increasingly higher-frequency transducers and other components, improved ease of use, enhanced cost-effectiveness, and the successful quest for creative medical applications and point-of-care markets.
These days, multiple companies are leading the charge in miniaturized guidance sensors and ultrasound system. Innovators in this space include Ultrasonix Medical Corp. (British Columbia, Canada), GE Healthcare, Esaote, Toshiba, and Hitachi.
In the past few years, newly emerging ultrasound segments have included procedure guidance for anesthesiology, breast surgery, and orthopedic surgery; aid in diagnosis and triage for intensive care and emergency medicine. These point-of-care applications, as well as price-performance and application-specific tools are driving the expanded use of ultrasound.
Applications supporting various medical specialties are continuing to emerge. These include guidance for nerve block procedures (anesthesiology), vascular access deep within a patient’s body (interventional radiology), and breast biopsies, injections, aspirations, radiofrequency ablation and—eventually—gene therapy.
Both increased miniaturization and improvements to front-end electronics lead to reduced size of systems, lowered cost of units, and boosted performance, says Laurent Pelissier, president of Ultrasonix. New technologies predicated on 3D guidance and improved sensors show promise to assist in a wide range of applications.
Biopsy Guidance Device Opens a View to New Technologies
Guidance for biopsy is commanding attention, thanks in part to Ascension Technology’s development of 0.9 mm and 0.55mm, six-degrees-of-freedom (DOF) sensors. Ascension Technology and CIVCO Medical Solutions developed the proprietary needle guidance system for ultrasound platforms, providing them with a freehand guidance capability. Combined with sophisticated visualization software, the system enables concurrent tracking of ultrasound scan planes and the distal tip of a needle, allowing real-time visualization of needle position and patient anatomy with optimal accuracy.
Until recently, ultrasound was unable to independently ensure that either a biopsy needle tip or ablation probe electrodes would accurately penetrate lesions. However, sensor guidance, aided by pre-operative imaging, eliminates the guesswork by simultaneously tracking the transducer and needle tip in 3D.
Today, systems are poised to move well beyond biopsy into more advanced clinical applications, enabling ablation of malignancies and benign lesions, nerve blocking to inhibit pain, and deep venous access to facilitate multiple therapies. Additionally, procedures such as endoscopic fine-needle injection for gene therapy are on the horizon.
The technology facilitates the use of multiple modalities during procedures, allowing anatomic and functional imaging to be combined and functional or metabolic information to be used for real-time feedback during procedures.
Real-time feedback should improve a physician’s ability to carry out procedures, says Bradford Wood, MD, director of the Center for Interventional Oncology and chief of interventional radiology, National Institutes of Health Clinical Center. “The specific settings in which it will be most beneficial, useful and practical are still being defined,” he says.
GE’s LOGIQ E9
Michael J. Washburn, principal engineer with GE Healthcare’s Ultrasound Division, says sensor technology that is integrated in the company’s E9 platform has advanced as new capabilities have been added, such as volume navigation.
Needle tracking and fusion imaging are a useful utility for clinicians, Washburn says. Washburn points out that clinicians can import information from prior exams and correlate it directly to a real-time ultrasound procedure. “From a continuity of care standpoint, you want to bring that information right into your exam and build off it as opposed to just taking a look at it over at the PACS station and starting anew,” he says.
According to Washburn, E9 capabilities help facilitate diagnosis, biopsy, treatment monitoring and follow-up. Specifically, sensors enable further analysis and treatment of liver lesions, including biopsy and RF ablation of tiny lesions detected using the contrast procedure MR EOB; cryoablation of kidney lesions; and navigation to vascular aneurysms, blockages, or leaks for further evaluation of anatomy and dynamic blood flow.
Practitioner Reviews
Sensor-guided ultrasound has shown to result in fewer complications, less surgical time and expense, increased physician confidence, abbreviated patient discomfort, less anxiety and faster recovery compared with standard treatments.
Hisham Tchelepi, director of ultrasound, Department of Radiology, Wake Forest University School of Medicine finds sensor-guided ultrasound particularly useful when the needle angle approaches 90° to the ultrasound beam and when targeting lesions high in the dome of the liver, where conventional probe guides may be limited.
Tchelepi says it improves the confidence of radiologists who feel intimidated by ultrasound procedures when attempting freehand techniques. “It works best when performing procedures off plane, such as when the needle can’t be seen with confidence,” he says.
William S. Rilling, director of vascular and interventional radiology at the Medical College of Wisconsin, uses the technology primarily for renal and liver tumor ablation procedures. He, too, thinks sensor-guided ultrasound will improve outcomes as the technology matures. “The entire field of percutaneous tumor ablation is evolving with improved planning, guidance, monitoring, and endpoint determination,” he says. “Technologies such as this will hopefully translate into improved patient outcomes.”
Michael D. Beland, director of ultrasound at Rhode Island Hospital, uses sensor-guided technology to perform biopsies in the liver and on soft tissue masses. He sees future utility in training of residents and sonographer. Regarding present usefulness, he states: “It has allowed increased confidence during certain biopsies and permitted some to be performed ultrasonically that would have gone straight to CT. Real-time image fusion across multiple modalities is a breakthrough technology,” he says.
Steven K. Wagner is a freelance writer based in Claremont, CA.
About the Author(s)
You May Also Like

.png?width=300&auto=webp&quality=80&disable=upscale)
