Safe for the Sick (and Everyone Else, too)
Protecting patients and care workers from danger in the hospital is no easy task.
April 1, 2009
MDEA 2009
As movie mogul Samuel Goldwyn once observed, “a hospital is no place for the sick.” Although meant as a joke, his statement has taken on a frightening reality as we learn more about bacteria with antibody resistance, surgeries performed on the wrong side of the body, and bedsores so severe that patients can lose limbs.
Luckily, protecting people at risk for such problems takes shape in various ways. Device designers are taking steps to incorporate antimicrobials into devices and searching for ways to provide faster, more-personalized diagnoses. They are even looking for simple ways to provide an indication in CT scans, to ensure radiologists look at images right side up.
Some of the solutions are complex, some are simple, but all of them are groundbreaking, which is what makes them stand apart from the crowd. It also makes them worthy of a Medical Design Excellence Award.
A Farewell to HACs
Preventing infections in hospitals is of critical concern to patients. Nosocomial, or hospital-acquired conditions (HACs), are particularly challenging because they usually prey on immune-compromised patients. And the problem is even more urgent because CMS recently issued its policy not to provide reimbursement for certain HACs.
|
Preventing and treating pressure ulcers has been a difficult process. The Envision system from Hill-Rom is specifically designed to stop the causes of such ulcers. |
Envision E700 Wound Surface. For example, one condition Medicare will no longer cover is bedsores. A decubitis or pressure ulcer forms when an area of skin breaks down as a patient stays in one position for too long. Constant pressure against the skin reduces the blood supply to that area, and the affected tissue dies. The ulcer starts as reddened skin but gets progressively worse, forming a blister, then an open sore, and finally a crater. The most common places for pressure ulcers are over bony prominences like the elbow, heels, hips, ankles, shoulders, back, and the back of the head.
The Envision E700 Wound Surface from Hill-Rom Co. (Charleston, SC) is a system that addresses the five key factors affecting pressure ulcer healing: pressure, shear, friction, patient immobility, and microclimate management. Helping this patient population is something Hill-Rom has always emphasized, explains Terry Mirabella Moran, director of critical-care marketing. She says the company has conducted pressure ulcer analyses for almost 20 years. “The CMS policy gave visibility to the problem—and the market is seeing the need for hospitals to take it much more seriously.”
The designers specifically focused on patients who currently have pressure ulcers or are at high risk for developing them. Envision's specialty surface incorporates sensing and weight-based pressure redistribution technology. It has multiple layers of 3-D fabric encased in a shear liner that shifts along with the patient. The effect minimizes shear and friction during patient movement. In addition, a unique algorithm automatically adjusts the seat and back to reduce shear and friction when the head of the bed is raised. Just beneath the patient is an environment that wicks excess heat and moisture from underneath and vents to the head end of the mattress. Vertical air cells in the foot section act independently to optimize immersion and envelopment of the patient's heel, which is particularly vulnerable. The system also has programmable reminders for timed assessments and alarms if the patient unexpectedly gets out of bed.
“There are risk-related reasons and some clear financial implications to the hospital that drive the need to enhance patient outcomes through new product development,” says Moran. “We strongly believe that helping the patient—and the caregiver—is vital.”
|
Esterline designed the Medigenic keyboard with an emphasis on creating a flat, cleanable surface, but also focused on tactile feedback for users. |
Medigenic Infection Control Keyboard. Easing the way for caregivers doesn't just include patient interaction. Caregivers are under stress to ensure that their workspaces are sanitary. Multiple users touch computer equipment on a daily basis, but simple objects, like keyboards, are often overlooked. Juror Gail Baura says, “Until recently, many people took it for granted that the sterile field remained sterile.”
As juror David Yadin puts it, “[The keyboard is] one of the least attended-to products in the healthcare system and yet it is depended upon to enter critical healthcare information data.”
The colonization rate of potentially pathogenic microorganisms is greater on keyboards and mouses than on any other surface in an ICU, according to the Journal of Clinical Monitoring and Computing.
Randy Noland, director of marketing at Esterline Advanced Input Systems (Coeur d'Alene, ID), highlights the danger. “A caregiver can pick up bacteria from a keyboard that is contaminated with, for example, methicillin-resistant Staphylococcus aureus (MRSA). Some colonies have been shown to survive up to 24 hours on a keyboard,” he says. The number of deaths caused by cross-contamination is more than car crashes and breast cancer combined, says Noland.
Providing sterile keyboards is not a new concept, but doing it well has been a challenge. Juror Steve Wilcox says, “Historically, the options were either an easily cleanable (typically membrane) keyboard that wasn't particularly usable or a usable keyboard that wasn't particularly cleanable.” However, Esterline has provided an elegant product to combat those flaws.
The Medigenic Infection Control Keyboard features a sleek design that emphasizes quick cleaning with common hospital-grade disinfectants. Noland explains that the impetus came from the University College London Hospital. “They told us they couldn't clean a conventional keyboard, and that the supposedly cleanable keyboards didn't meet their needs.”
So Esterline went to work designing a keyboard that could be flat, cleanable, and usable. But, recalls Noland, the company wasn't alone. “We found out later that the [hospital] contacted about three other companies. But we won the contract because our keyboard is the only one that is totally flat and still has a nice tactile feel to it, so that users don't lose speed and accuracy.”
The keyboard and mouse have a seamless design, with no crevices, to reduce risk of bacterial cross-contamination. An alert system notifies users when the silicone rubber keyboard cover requires cleaning. Backlit keys make the keyboard usable in low-light areas, and the design promotes tactile key response.
Jurors responded to the product's well-marked keys, general connectivity, soft touch, and feedback system. “This keyboard is unique in the way it incorporates user behavior in its design,” Yadin says.
Noland says hospitals will soon begin to see the Medigenic technology in other medical equipment. “Our main business is to manufacture custom controls. So we expect to be able to apply the technology of the keyboard to ultrasound, magnetic resonance imaging, and computed tomography control panels.”
Brave New Diagnostics
In vitro diagnostic (IVD) products made up a significant portion of MDEA winners this year. Juror Mark Vreeke believes that this is because “the medical community is beginning to recognize the value of diagnostics and more money is going into product development.” Increased personalization in medicine is a long-promised innovation and one of this year's winners is a first in that market.
More commonly, the winning products in this category placed emphasis on making tests more rapid and automatic. The designers of these devices know that the value of IVDs depends on making tests that are easy to perform and yield results faster than ever before.
|
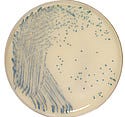
The Spectra MRSA plated medium helps caregivers quickly diagnose the hospital acquired infection, enabling aggressive treatment to prevent spreading. |
Spectra MRSA Chromogenic Plated Medium. Infections in hospitals can spread rapidly, even with precautions taken by hospital staff. For that reason, hospitals need to be able to quickly and efficiently test all patients continuously for certain infections. The annual cost of treating patients that contract MRSA is estimated to be $3.2 billion to $4.2 billion. Aggressive prevention measures can only begin, however, if low-cost and simple screening is made available. The Spectra MRSA by Thermo Fisher Scientific, Remel Products (Lenexa, KS) aims to provide such screening. The diagnostic test is ready to use and designed to save costs and labor.
Juror Steve Wilcox says, “The Spectra MRSA plate provides a simple, elegant solution to the real problem of MRSA infection that hospitals are facing.”
The rapid-screening medium uses chromogenic technology to detect phosphatase activity. Although many bacteria produce phosphatase, nontarget organisms are inhibited by antibiotics and other agents contained in the medium. The medium also contains compounds that encourage the production of a MRSA pathogenicity marker, ensuring expression of the phosphatase enzyme. MRSA grow as blue colonies on the medium within 24 hours, making aggressive prevention and treatment possible for patients. The medium has a positive predictive value of 98.1%, according to the company.
Vreeke says that the key to the Spectra MRSA is that it encourages screening as a standard practice for hospitals. He says that because the product is low cost and quick, it can be incorporated into the hospital work flow.
|
The eSensor XT-8 tests for warfarin sensitivity using genomic data. Such diagnostics are a long-promised advance in the IVD market. |
eSensor XT-8 System for Warfarin Sensitivity Testing. Another winner from the IVD category is a product that fills a significant need for compliance to medication regimens. And it does so using intriguing new technology. The eSensor XT-8 system for warfarin sensitivity testing from Osmetech Molecular Diagnostics (Pasadena, CA) is one of the first to be offered in the field of personalized medicine, says Vreeke. “The eSensor XT-8 is one of the few commercial examples in which molecular diagnostics is making forays outside of the research and cancer markets,” he says.
Having a genetic IVD that specifically tests for warfarin sensitivity is important because of the extreme risk of adverse events that come from overdosing. The anticoagulant is used to prevent heart attacks, strokes, and blood clots in veins, arteries and lungs. However, severe bleeding events occur in 70–100 for every 1000 patients on the drug. “It is among the top three drugs causing adverse events requiring hospitalization or emergency room visits,” says Robin Liu, director of device technology at Osmetech. Warfarin has shown distinct correlation between sensitivity between the drug effect and specific genotypes, explains Liu.
The eSensor uses polymerase chain reaction (PCR) and electrochemical detection microarray technology to genotype the alleles that correlate with therapeutic warfarin dose and with the frequency of adverse effects from overdose. “The fact that it is electrochemical is important because most microarrays are optical. Our device is more robust because it doesn't have optical parts,” Liu says. Pathologists can use the report to identify high-risk patients, and physicians use the data to determine dosage.
The eSensor system is unique in its design, something several jurors admired. The system consists of a disposable cartridge and reagents. It is a modular design with a base and up to three cartridge towers that contain up to 24 cartridge slots. The base module has an embedded computer to communicate with each tower. The disposable cartridge is a printed circuit board (PCB) microarray chip with a microfluidic component. “PCB is inexpensive and helps us keep costs down for the product,” Liu says.
The PCB chip contains 72 gold-plated working electrodes. Each electrode is a DNA microsensor coated with specific single-strand DNA molecules (capture probes) with unique sequences. A proprietary surface chemistry involving a self-assembled monolayer that includes presynthesized oligonucleotide capture probes is employed. Moreover, a proprietary chemistry involving the signal probe containing electrochemically active ferrocene labels is used for DNA detection. The microfluidic component of the cartridge is composed of an injection-molded polycarbonate plate and a unique multilayer laminate that is cut using laser micromachining. The laminate forms a diaphragm micropump, check valves, and the fluid circulation channel, which enable repeated circulation of the sample solution over each electrode.
The result of such complex technology is a simple, effective test that Wilcox says “makes testing for warfarin sensitivity simpler, more intuitive, and more accessible than it was previously.”
Liu says the microarray technology enables the user to detect multiple targets using a single device. He says that future plans for the modular device include testing for cystic fibrosis and upper respiratory diseases.
The Right Stuff
A safety check doesn't have to incorporate revolutionary technology design to be worthy of an award. Simple designs can solve significant problems. And a device that takes away the risk of operator error is a significant way to ensure patient safety. One device winner caught the eyes of the judges because of its straightforward approach to preventing wrong-side surgeries.
|
Identifying the right-hand side of a CT image using the Accu-Right removes the risk of operator error for image orientation. |
Accu-Right CT Marker Device. The Accu-Right, manufactured and submitted by Accu-Right Correct Side Solutions LLC (Los Angeles), helps operators determine the right-hand side in computed tomography (CT) images in a simple manner. It is as easy as putting on a pair of glasses. Plastic goggles are affixed with an extruded rod shaped like an “R.” The patient wears the goggles during a CT scan. The rod is made from polyvinyl chloride, which shows up as part of the final image. “That was one of the most difficult parts to design,” says Kevin Mackay, president of the company. He explains that the “R” could not be injection molded and the original design could not be extruded. “We only found success with extrusion once we removed the circle around the ‘R' from the first design draft.”
The goggles are injection molded from polypropylene and significant attention was given to ensuring that they cannot be used incorrectly. For example, the “R” rod can only affix to the right side of the goggles. A hump on the bridge of the nose prevents the user from putting the device on upside down, and engraved lettering on the front also protects against incorrect placement.
This single-use recyclable CT accessory may reduce wrong-side surgery. “Image reversal is a serious problem and can lead directly to wrong-side surgery,” says Bill Hyman, one of the MDEA jurors. “The existing methods for adding left-right designation are not often definitive and in some cases rely on the human operator to provide the correct designation. This is not a robust process from the perspective of avoiding use error.”
Mackay, who is also a radiologist, says the risk of wrong-side surgery is significant. He says that when he shows the device to physicians they have three comments right away. “The first one is ‘Wow, what a great idea;' second, they tell me a story about a wrong-side surgery they witnessed or know about; and third, they ask ‘When can I use it?'”
According to Hyman, Accu-Right's “simple but not simplistic” design is both effective and affordable. “The judges this year noted with respect to several submissions that high cost and high complexity did not necessarily equate to award-winning design,” he says. “Low cost and low complexity could and should lead to an award when a real solution to a real problem is presented. The Accu-Right is such a product.”
Conclusion
Many of the devices that made up this year's MDEA winners had clear emphasis on the safety of the patient. Jurors were impressed with the forward-thinking designs that emphasized safety for healthcare workers, too.
Safety is not just about better patient outcomes, however. It's also about reducing the financial burdens of healthcare for everyone. A patient protected from HACs leaves the hospital sooner and hospitals don't have to worry about how to pay whatever insurance won't cover. A patient pretested for drug sensitivity is less likely to require emergency room treatment. And a disposable product that provides a simple safety check protects hospitals and patients from the expense of a wrong-side surgery. New technologies, proper cleaning mechanisms, specific and quick diagnoses, and simple safety checks reduce costs, as well as patient risks.
The ultimate goal, of course, is to help patients get better. This year's MDEA winners have that goal firmly in hand.
Heather Thompson is managing editor of MD&DI.
Copyright ©2009 Medical Device & Diagnostic Industry
About the Author(s)
You May Also Like