Robotics and Electronics Research Aid in Building "Smart" Prostheses
Medical Device & Diagnostic Industry MagazineMDDI Article IndexOriginally Published January 2001R&D HORIZONSThe next generation of prosthetic limbs will incorporate technology that provides a more natural gait and greater comfort and efficiency, and may restore certain sensory functions.William Loob
January 1, 2001
Medical Device & Diagnostic Industry Magazine
MDDI Article Index
Originally Published January 2001
William Loob
A complicated assemblage of pneumatic tubes and metal rods hangs in the BioRobotics Lab at the University of Washington (Seattle). It vaguely resembles a human arm that has been stripped of its skin to reveal the underlying musculature and skeletal structure. And that is exactly how it should look, according to the team of research engineers and scientists who built the contraption. A fully functioning version of the machine is the goal of the lab's Anthroform Arm Project—one of two current research efforts aimed at developing robotic components that are capable of imitating biological systems.
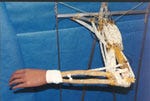 The Anthroform Biorobotic Arm uses McKibben artificial muscles, bundles of pneumatic actuators that exhibit many properties found in human muscles.
The Anthroform Biorobotic Arm uses McKibben artificial muscles, bundles of pneumatic actuators that exhibit many properties found in human muscles.
Although the original intent of the project was not to improve on existing prosthetics technology, the effort could someday lead to development of an artificial arm that enables an amputee to regain the full range of motion offered by a natural arm. The lab's director, Blake Hannaford, PhD, states that, in this case, creating a more effective robotic system required the engineers to learn from other technical fields. One practical benefit of such an interdisciplinary approach might well be a more efficient prosthesis design.
Increased efforts to address the problems associated with unexploded land mines in some parts of the world have focused attention on the field of prosthetics and orthotics. Greater consciousness about amputee quality of life has also promoted research efforts to develop a new generation of products. Some of the technology being explored for use in advanced prosthesis designs is being drawn from disciplines outside of conventional orthotics and prosthetics development.
The complexity of human limb movements has posed difficult challenges to prosthetic-limb designers. Restoring the functions of a natural arm or leg has been difficult, and most designs for artificial limbs are generally able to perform only the simplest functions of the missing extremities. The technologies now in development are expected to address such limitations in conventional systems. In addition, specialized prosthesis designs are emerging to meet the needs of amputees who are involved in a range of physical activities.
One of the persistent problems of prosthetics development is designing a suitable method for attaching the prosthesis to the remaining stump. The goal is to maximize comfort yet retain firm and stable contact for controlling the limb. Use of rigid materials means that the fit of a prosthesis will vary over the course of the day as the stump tissues swell or shrink. The result is often discomfort and reductions in controllability. Sores can also become a problem and may limit the length of time an amputee can wear the prosthesis.
Prosthesis designs can have a significant effect on an amputee's normal gait and the physical responses to prosthetic limbs. Researchers analyzing the gait of patients using prosthetic legs have found that amputees often compensate for the loss of their natural walking gait with unnatural body movements to accommodate the prosthesis. Tailoring a design to restore more-natural movements for the amputee not only would increase comfort, but also could actually reduce fatigue.
USING SMARTER MATERIALS AND COMPONENTS
Prostheses can be fabricated from materials selected to provide characteristics suited to the specific mechanical requirements of a given activity. An amputee often needs to switch between different prostheses, however, to engage in different activities. Some firms are incorporating "smart" materials and components into prosthesis designs in an effort to expand the range of environments in which a prosthetic device will perform most efficiently.
A prosthetic leg developed for above-knee amputees by Biedermann Motech (Schwennigen, Germany) uses an array of sensors in the artificial knee component to detect force and moment exerted on the prosthesis and the angular position of the knee joint. The mechanism also includes a damping device filled with a magnetorheological fluid that can adjust rapidly to changes in external forces. Input from the sensors and software algorithms control the damping qualities of the device. The fluid, which was developed by Lord Corp. (Cary, NC), is designed to change consistency—from a fluid to a near-solid state—in response to the strength of a magnetic field applied to it. According to the company, the time required to react to changing forces is 20 times faster than systems that use passive fluids. Such results more closely match human neural response times than hydraulic mechanisms with motor-controlled valve systems, according to the firm.
ROBOTICS BASED ON BIOLOGICAL MODELS
Development of systems that emulate biological models promises to yield significant advances in prosthetics technology. Efforts to mimic human anatomy with mechanical systems at the BioRobotics Lab have focused on the use of actuators bundled into what is called the McKibben artificial muscle. The pneumatically operated actuators provide a high force-to-weight ratio, the researchers indicate. In addition to the arm project, the lab is engaged in developing a prototype of a lower-limb prosthesis that is also powered by these actuators.
"We started with the robotic arm development project, and prosthetics is a natural application for such an arm," Hannaford says. "We wanted to see how far we could go with this idea." The early work on the project, which was focused more on robotics, led the lab's team to seek out medical researchers working with prostheses. The lab is also collaborating with the Veterans Administration Medical Center in Seattle to develop potential applications of the system for below-knee amputees.
Researchers at the BioRobotics Lab became intrigued by the physical energy requirements of conventional prostheses. "We learned that for an amputee with a conventional prosthetic, the rest of the body is compensating with energy: The amputee is working harder to walk at the same pace as a normal person." A power-assist system capable of replicating the function of natural muscle seemed to be a logical solution to the problem, Hannaford explains. "We thought that the gait of a prosthesis wearer would be more natural if we could replace some of the power of the lower-leg muscles." The team is still building a functional prototype of the powered prosthetic leg, but the main design effort is complete.
After the working prototype is finished, Hannaford says, the project team will move on to the next phase. They will assess how well an amputee adjusts to using this type of device and whether it can save energy for the prosthetic wearer. "We still need to take measurements and ask: 'What does an amputee's gait look like using an active limb replacement, versus how he or she uses a passive prosthetic?' and 'How much energy is the amputee using?'"
The development of a workable power-assist system would be a significant advance in the state of limb-prosthesis technology. The artificial muscle is easy to make, Hannaford says. The amount of strength per unit of weight and area is within a range to make the mechanism practical in this application. "It is actually a little stronger than human muscle, and the weight is comparable to the natural muscle mass." The bundle of actuators is capable of equaling the power supplied by the natural muscles that move the foot at the ankle joint. Hannaford admits, however, that the actuator bundle must also compensate for the weight of the compressed-air source. Also, the artificial muscle has a shorter range of motion than human muscle.
CYBERNETIC SYSTEMS
Researchers at Sandia National Laboratories (Albuquerque, NM), working in collaboration with engineers at the Russian nuclear weapons lab at Chelyabinsk-70 and the Seattle Orthopedic Group (Poulsbo, WA), are taking a more inclusive approach to addressing the most common problems for amputees. The international research team began a project this year to develop a prosthetic leg capable of adjusting itself to an amputee's gait, and of adapting to changes in the stump shape caused by tissue swelling.
 Sandia's synthetic lower limbs are expected to provide the foundation for the next generation of prostheses.
Sandia's synthetic lower limbs are expected to provide the foundation for the next generation of prostheses.
Sandia is developing the set of sensors and microprocessing chips that will provide information to the "smart leg," then calculate the optimum movement of its components to support the walker's gait. The system will be capable of altering the wearer's gait in response to changes in terrain.
Like Hannaford's group, the Smart Integrated Lower Limb Project will focus on reducing the energy an amputee will need to exert to walk with a prosthesis. The smart leg will be designed to simulate the human gaits used on uphill and downhill slopes, or on less-predictable and irregular terrain.
One set of sensors placed along critical points in the prosthesis components will feed data to microprocessor-based Controls used to govern hydraulic joints and piezoelectric motors that power the ankle- and knee-joint mechanisms. A second group of sensors in the leg socket will enable the device to compensate for any changes that occur in the diameter of the stump over the course of a day. Designing the prosthesis with a self-adjusting socket for attachment to the stump is a major goal that researchers believe will enhance overall efficiency. Not only are pressure sores a nuisance associated with lower-limb prostheses, discomfort can affect the wearer's physical posture and gait. Researchers expect the complement of improvements in performance to extend the effective time of use for leg prostheses.
"The majority of lower-limb prosthetic devices are based upon passive technologies," says Dave Kozlowski, a Sandia robotics specialist. Without powered systems to operate moving parts, passive prostheses rely on inertia to open the knee joint as the thigh moves forward so that the shin can then swing forward. The amputee must generally wait for the assembly to lock into its new position before the prosthesis can support the body as it moves forward.
This series of functions does not allow for a natural gait, Kozlowski explains. Without powered components, prosthetic legs "require far more energy for amputees to cover the same distance as nonamputees." Achieving proper limb motion will ease the physical effort of using an artificial leg—rather than draining energy from the wearer, he says.
One of the more difficult challenges of the project is developing a power source that is light enough to be practical, yet adequately robust to operate all of the required systems, according to the group. The Sandia researchers estimate that a marketable version of the system may be developed within about two years.
IMPROVING COMMUNICATION WITH PROSTHESES
The user's ability to control a prosthetic limb has been a particularly difficult problem to overcome with upper-limb prostheses. The range of motion required for arms, hands, and fingers involves the use of a complex set of variables that must be addressed by prosthetic mechanisms, and a correspondingly complex control interface to communicate with the device and direct its movements.
Animated Prosthetics (Greensboro, NC), a company specializing in prosthetic-control circuits, has developed systems to allow amputees to exert myoelectric control of hand and wrist movements in the prosthesis. The firm's Animation Control Systems circuits are based on use of different algorithms to respond to myoelectric signals from a patient's stump. The circuit response depends on the strength of the signal that is received. Gaining conscious control over the minute electrical signals generated by the muscles can be a difficult task for amputees to learn. To facilitate learning, the company designs its circuits to opt for a simpler operational algorithm to control the prosthesis when the signal is weak, as it is when the patient is still learning to regulate the signals sent to the device. Under those conditions, for instance, the circuit controls the grasping function of the hand with a simple, open-and-immediately-close operation. As the amputee learns to control the signals better, the algorithm adapts to keep the grasping appendages open until it receives a close command.
 The Edinburgh Arm System uses self-contained modular actuators.
The Edinburgh Arm System uses self-contained modular actuators.
Researchers are working on more advanced interfaces, however, which will be capable of returning full control to the patient. A number of research groups are exploring development of direct neural interfaces that will link the thought of an action with a signal that can be directly interpreted by a robotic device. One such project currently being conducted at the Georgia Institute of Technology's Biomedical Interactive Technology Center (Atlanta) is investigating whether signals recorded from micromachined electrodes implanted in the motor cortex can be reproduced to instruct robotic systems to prompt the movements associated with a conscious thought of the corresponding actions.
Neural signals associated with defined arm and hand movements are processed using pattern recognition techniques to determine the intended movement of an individual's arm. The same signals are then used to instruct a robotic arm to move according to control parameters derived from the neural data. Researchers at Emory University (Atlanta), who are collaborating in the project, have tested the system on a group of rhesus monkeys. Project funding from the NIH Neural Prosthesis Program is supporting the research and the development of similar technologies.
RESTORING SENSATION ARTIFICIALLY
An intriguing application of sensor technology is being used to feed information back to the amputee. Two systems invented by John Sabolich at his lab, Sabolich Research and Development (Oklahoma City), are designed to restore an amputee's temperature sensitivity through a prosthetic arm and pressure sensitivity through a prosthetic foot. The Sense of Feel Sensory System connects a pair of pressure transducers in the sole of an artificial foot to a circuit that conveys a signal to electrodes in the leg socket where it contacts the skin of the stump.
The circuit delivers a "tingling" sensation to the skin, which varies in amplitude corresponding to the force detected by the transducers. The ability to sense the difference in signal strength between the front of the foot and heel enables the patient to learn to interpret whether body weight is balanced over the foot. In the system developed for artificial hands, temperature sensors deliver signals corresponding to a hot or a cold sensation as interpreted by an onboard microprocessor. Both systems are being tested currently on amputees. Sabolich states that new patients are generally able to begin interpreting the signals as the proper sensations after only a few minutes of use.
CONCLUSION
Only a few years ago futurists and science fiction writers speculated about the potential of smart prosthetic devices to improve the quality of life for amputees. They visulaized the promise of creating prosthetic mechanisms capable of more naturally emulating the appearance and function of human limbs. Today, the development of advanced prostheses is benefitting from increased collaboration between old competitors, and by the use of new materials technology, as well as emerging processing and mechanical concepts.
FORMER COLD WAR OPPONENTS COLLABORATE ON ARTIFICAL KNEE DEVELOPMENT Efforts to develop advanced prosthetic systems are clearly benefitting from the rapid changes occuring in the materials and computing sciences. The end of the Cold War and the refocusing of the nation's technological capabilities away from weapons research and toward helping the victims of war has become a significant factor in the development of prosthesis technologies. In 1999, a unique collaboration was initiated between nuclear laboratories in the United States and Russia. The arrangement between Sandia National Laboratory and the Russian laboratory known as Chelyabinsk-70 called for the two former adversaries to work together on the joint development of advanced prostheses. One of the driving factors behind the collaborative effort was to provide advanced treatment options for victims of land mines. "Someone in this world loses a limb to a land mine explosion every 20 minutes. Our work, though only remedial, will help land mine survivors and other amputees," said Sandia chemist and project leader Mort Lieberman when the project was announced. He added that, "We will have created the world's biggest research center for lower-limb prostheses in a Russian laboratory." Lieberman also serves on the executive board of the International Institute for the Prosthetic Rehabilitation of Landmine Survivors. The first collaboration, aimed at development of an artificial foot, resulted in significant improvements in motion over currently marketed prosthetic feet. A subsequent project, a mechanical polycentric knee, was based upon Sandia's electronic expertise and Russian materials knowledge. The partners' efforts were focused on creating, respectively, the brains and shape of the knee. "The work is a good fit with the capabilities of both labs," according to Lieberman. "It involves stress analysis, mechanical testing, reliability testing, microprocessor control, and materials analysis."
Under the collaborative agreement, the Ohio Willow Wood lab (Columbus, OH) was responsible for defining the requirements for parts and for performed final laboratory and clinical testing. The Russian lab designed the titanium housing, and Sandia's robotics researchers designed the knee's internal workings and electronics. The project received approximately $1.4 million in initial research and development funding. The researchers emphasize that a knee must offer a variable speed of response. It must also lock to keep the wearer from falling when standing. They explain that the knee is more than a simple hinge. It must offer adequate control and stability to the wearer. The ongoing U.S./Russian project is also expected to help the prosthetics industry as a whole. The industry has typically been dominated by small companies, which have relatively limited support. Most often, they lack the necessary resources to perform the type of testing that is possible at the nuclear laboratories. The current research project, development of the "smart" leg microprocessor-controlled prosthetic to help lower-limb amputees obtain a more natural gait, is only one of the proposals that have been submitted by the Sandia and Chelyabinsk-70 researchers to various funding organizations. Other proposals deal with the creation of sockets capable of adjusting to the swelling and shrinkage of an amputee's stump during the course of the day and knees that can help prevent falling when a wearer stumbles. |
William Loob is a medical writer living in Brooklyn, NY.
To the MDDI January 2001 table of contents | To the MDDI home page
Copyright ©2001 Medical Device & Diagnostic Industry
About the Author(s)
You May Also Like


