April 1, 2015
One day, we'll have little need for many medical devices if a University of Louisville professor is right.
Brian Buntz
|
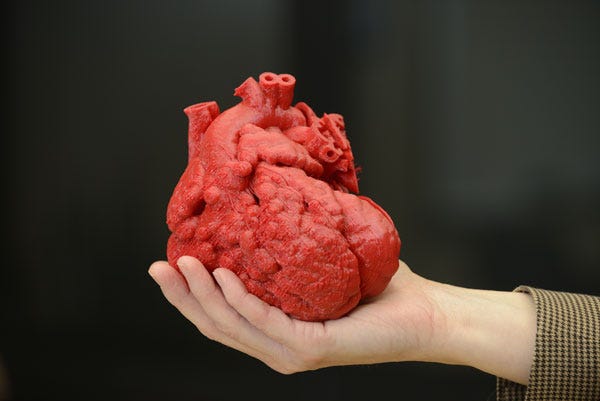
The heart model developed at the University of Louisville is used for surgical planning. |
"We've been using medical devices for decades in order to keep our tissues and organs going until we figure out a way of reconstructing those tissues and organs," University of Louisville professor Stuart Williams said at the Bay Area Biomedical Device Conference, held March 31 at San Jose State University. "Medical devices hopefully will just be bridges to biological solutions."
Having 3-D printed complex organs might be a reality in our lifetimes. In fact, Williams has the goal of creating a 3-D printed heart within a decade's time. "I believe the heart is going to be one of the easiest organs to print because it has very few types of cells and a relatively simple function--it just has to have a contractile capability," he said. "The brain would be the most difficult organ to print because we will argue over 1000 years whose brain to use as a model," he joked. Organs such as the liver and kidney would also be challenging to print, falling somewhere in the middle of the heart and brain. "We can print hundreds of thousands of cells and create the form of a kidney but we don't know how long it will take to create a functional kidney," he explained. "That's why I want to go after the heart first. It is relatively simple and one of the easiest organs to transplant." (Note: He'll be delivering a talk titled "The realities and myths of building 3-D printed body parts" at BIOMEDevice Boston in May.)
While the idea of tissue engineering, or at least culturing organs, actually goes back to the work of Charles Lindbergh in the 1930s, we are just now on the verge of using stem cells to repair an array of health problems. "We are not quite there yet," Williams acknowledged, but research breakthroughs are being announced on a near daily basis, and clinical trials are being launched across the world to evaluate tissue regeneration.
"The hope is that stem cells will become everything that we possibly need as a replacement. We are going after absolutely everything. We want to take medical devices out of it and repair all of these tissues," he said.
To support that argument, Williams points to how far tissue engineering has already come. A company named Tissue Genesis (Honolulu, HI) has developed technology that can isolate tens of millions of regenerative stem cells in an operating room environment in an hour's time. In 2011, the company launched a clinical trial to test a stem-cell-coated vascular graft.
A year prior to that, The Economist ran a cartoon that suggested that 3-D printers could print out any organ a surgeon might need. "We are getting pretty close to that as these devices are starting to move into the operating room," Williams said.
Right now, 3-D printing has reached the stage of clinical use for certain applications, such as the production of custom anatomically correct heart models or vascular systems that are used by surgeons as a training aid.
|
In decades to come, we could have more advanced artificial heart technology than this plastic and metal model depicted in Star Trek: Next Generation. |
While printing a functional heart may sound like science fiction today, Williams said that perhaps even Star Trek doesn't boldly go where it should. "In a few hundred years, Jean-Luc Picard [in Star Trek: Next Generation] still gets a piece of plastic and metal to fix his heart. For God's sake, go and talk to your science fiction writers and tell them there is hope in regenerative medicine and cell-based therapy for the heart, too."
The biggest hurdle that still remains for the field is related to bioinks. "We are getting good at the isolation of cells, processing images, bioprinting, using glues and polymers--extracellular matrix and other materials, we understand additives, are getting much better at understanding growth factors. But putting them all together into a bioink and being able to print a structure that then develops to a kidney, a heart, a brain, or whatever it is, that's where the real problems exist," Williams said.
While it is already possible to create detailed models of the heart based on MRI or CT data, Williams recommended not holding too closely to the organ's original design. "The original design for a heart is flawed because it puts one major vessel into the left part of the heart. As we talk about printing a new heart, why don't we make a better design?"
Already, scientists can print vascularized tissue, making it possible to create heart valves and cardiac patches that can be surgically implanted and become fully functional with a short period of time. "Cells from the fat can be used to grow brand new blood vessels. We also find you can do that under in vivo conditions," he said.
Hear Williams speak in person at BIOMEDevice Boston, May 6-7, 2015. |
Brian Buntz is the editor-in-chief of MPMN and Qmed. Follow him on Twitter at @brian_buntz.
Like what you're reading? Subscribe to our daily e-newsletter.
About the Author(s)
You May Also Like