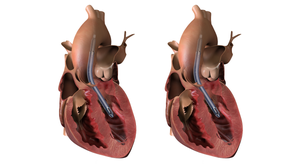
Abbott HeartMate 3 heart pump (left ventricular assist device) designed to help the heart pump blood to the rest of the body.
QA/QC
14 Deaths Connected to Latest Abbott HeartMate Recall14 Deaths Connected to Latest Abbott HeartMate Recall
Long-term buildup of biomaterials can obstruct the device, making it less effective at helping the heart pump blood.
Sign up for the QMED & MD+DI Daily newsletter.


















.png?width=300&auto=webp&quality=80&disable=upscale)


.png?width=300&auto=webp&quality=80&disable=upscale)
.png?width=300&auto=webp&quality=80&disable=upscale)


.png?width=300&auto=webp&quality=80&disable=upscale)
.png?width=300&auto=webp&quality=80&disable=upscale)
.png?width=300&auto=webp&quality=80&disable=upscale)
.png?width=300&auto=webp&quality=80&disable=upscale)
.png?width=300&auto=webp&quality=80&disable=upscale)
.png?width=300&auto=webp&quality=80&disable=upscale)

.png?width=300&auto=webp&quality=80&disable=upscale)
.png?width=300&auto=webp&quality=80&disable=upscale)



.png?width=300&auto=webp&quality=80&disable=upscale)
.png?width=300&auto=webp&quality=80&disable=upscale)


.png?width=300&auto=webp&quality=80&disable=upscale)