Winners of this year’s BMEIdea competition created medical devices to improve health in the developing world, provide faster relief for patients suffering from a common but painful ailment, and simplify a lifesaving emergency procedure.
June 20, 2012
The competition, put on by the National Collegiate Inventors and Innovators Alliance (NCIIA), judges biomedical devices submitted by teams of undergraduate and graduate students from across the country. The 2012 winners were announced in May at MD+DI’s Medical Design Excellence Awards Ceremony in Philadelphia.
|
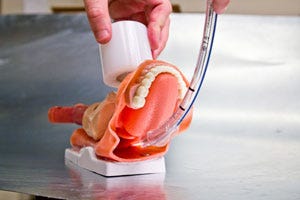
Cryopop could prevent cervical cancer deaths in the developing world. |
A team from Johns Hopkins University came away with the top award for CryoPop, a device for treating cervical cancer in patients in developing countries. Instances of the disease have fallen in places like the United States thanks to regular screening and vaccinations, but that’s not the case in the developing world, where almost nine in 10 cases of cervical cancer occur.
The three members of the team, which has incorporated under the name MoMo Scientific, met while earning master’s degrees at the Johns Hopkins University Center for Bioengineering and Innovation Design. As part of the program, the students spent three weeks in countries such as India and Nepal, where they learned about the challenges of treating cervical cancer in the developing world.
The standard of care device used for treatment there is a cryogun, which uses the expansion of carbon dioxide gas to cool a metal tip that ablates precancerous lesions in patients at risk of developing cervical cancer. But such devices are unreliable and difficult to fix due to their complex assemblies. The CryoPop also harnesses carbon dioxide to perform ablation, but it cools liquid carbon dioxide into a block of dry ice to freeze the cervix.
“This basically enabled us to make the device with just a couple of components that can be mass manufactured,” says team member Marton Varady.
The device consists of two injection-molded parts and can be fueled by carbon dioxide tanks used for carbonated soda, which are readily available in developing countries. Its low-cost components could mean a high profit margin for the device itself, says team member Shuja Dawood, but that’s not all the team was interested in accomplishing.
“Our return is not just financial, it’s a social return of saving lives,” says John-William Sidhom, who also worked on the project.
|
This device could help treat patients with small kidney stones in a urologists office. |
The second-place prize went to a device that could bring faster relief to patients suffering kidney stones. The vast majority of patients (85%) suffer from stones too small for current treatment methods and are thus sent home with narcotics to wait for the stones to pass naturally, an often painful process. Calcula Technologies, from Stanford University, has developed a minimally invasive device that enables urologists to treat kidney stones in a single office visit and without general anesthesia. The team declined an interview request from MD+DI.
A team from the Georgia Institute of Technology took third place with a device to aid the crucial but difficult process of airway stabilization in emergency patients. Laryngoscopes currently used to aid in the process can chip teeth and serve as vectors for disease, says team member Shawna Hagen. There’s also a steep learning curve for care providers. Nearly a quarter of first-time intubation attempts in emergency situations result in failure.
“The technology hasn’t changed in last 34 years,” Hagen says. “This was just an accepted difficulty within emergency medicine, and we saw a need to change that.”
She and team members Alexander Cooper, Elizabeth Flanagan, and W. Jacob Thompson, developed a device that uses a magnetic stylette and magnets placed outside of the neck to guide the assembly through the trachea and into the esophagus. Hagen says the single-use Magnet-Assisted Intupation Device, or MAID, will be cost competitive with current standard-of-care laryngoscopes and endoscopes, and it will cost drastically less than video laryngoscopes.
|
MAID is designed to simplify intubation. |
Now in its eighth year, the BMEIdea competition was conceived by the NCIIA and a number of university biomedical engineering departments as a way to prepare students for the task of bringing a medical device to commercialization.
“Students were going through four-year programs and learning great things about engineering and design, but they weren’t prepared for the full bredth of what it really takes to commercialize a biomedical engineering device,” says program director Humera Fasihuddin. “Our aim was to give them a crash course by way of a competition.”
Teams have increasingly been taking their projects beyond their competition, she says.
“What we’ve been noticing lately is that the students themselves are much more committed,” she says. “They know coming in that they’re going to pursue this and take it forward.”
All three of the 2012 winning teams plan to continue working in some capacity to bring their devices to market, she says.
About the Author(s)
You May Also Like