Stryker's Performance Solutions division is giving hospitals and patients more tools to improve care quality and to meet—or beat—Medicare target prices for hip and knee replacement surgeries.
August 5, 2016
Stryker's Performance Solutions division is giving hospitals and patients more tools to improve care quality and to meet--or beat--Medicare target prices for hip and knee replacement surgeries.
Through its Episode Performance Manager platform, Stryker's Performance Solutions offers hospitals data reports that they can use to cut costs and improve the quality of care.
Major orthopedics companies aren't sitting idly by as bundled payments and Medicare's mandatory Comprehensive Care for Joint Replacement (CJR) model impact their customers. Stryker's Performance Solutions business has been unveiling technology to help patients prepare for joint replacement surgeries as well as data analysis tools for hospitals looking to improve care and cut costs.
In July, Stryker's Performance Solutions (SPS) announced Episode Performance Manager, an expansion of its digital platform, to give hospitals actionable data reports pulled from analysis of CMS's raw claims data. A couple months earlier, the company also released its JointCOACH platform to give patients more information about the joint replacement procedures they are schedule to undergo.
MD+DI has previously reported on Zimmer Biomet's Signature Solutions offering with tools to help hospitals and patients cope with changing business models.
Brian McCrone, MBA, vice president of SPS, said, "We realized that [customers] aren't prepared to manage the risks associated with this change or how they're going to manage getting the data and doing something with it . . . We created this to try to simplify their life and help them be prepared to navigate the change."
SPS is also sharing risk with some of its customers in its role as a convener. "We're helping those customers manage their entire episode and we're going at risk with them," McCrone added.
Start planning your fall schedule now. Register for the MD&M Minneapolis Conference, September 21-22. |
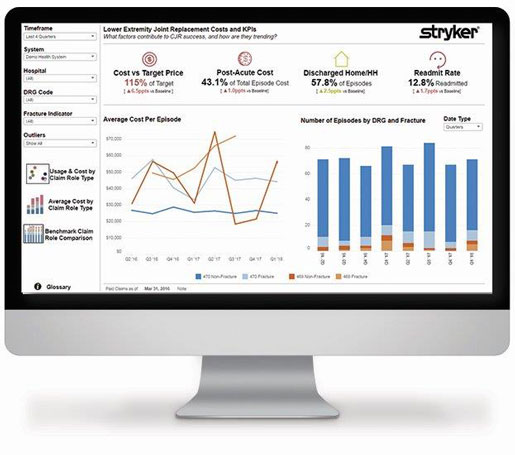
The Episode Performance Manager
The Episode Performance Manager platform gives hospitals the data on episode costs that they need, without having to wade through the raw data from Medicare. The goal is to give hospitals enough insight into the factors behind their current care quality and episode costs to enable action and improvement. "Data is only as good as what you do with it," McCrone said. "We're going to help [hospitals] look at data in a way they never really thought to look at the data. Then we're also going to develop a plan with them to use the data to impact their care pathway to allow them to be successful."
The SPS team walks customers through the large amount of data available to them. First up, hospitals might look at their current episode cost versus the target price that has been determined by CMS. Jordan McInerney, MHA, program manager in SPS, showed MD+DI the multitude of data points available. Hospitals can see what percentage of total episode cost is spent on post-acute care (a key focus area for reducing costs), what percentage of patients are discharged to their homes or home healthcare settings, and the readmission rate. These metrics are compared to the hospital's baseline data and can be viewed as a trend line too.
These metrics can be useful in a number of ways, including motivating physicians by showing them their stats versus their colleagues' stats. "Surgeons are extremely competitive people. The best way to drive change is to line them up beside each other," McInerney said. "We're just trying to facilitate the sharing of best practices."
In addition to many other data points, hospitals can also track where their joint replacement patients go for recovery after the procedure and evaluate cost and quality data on each facility. Then, they can have physicians change where they send their patients upon discharge and also work with facilities to reduce large discrepancies in care costs.
|
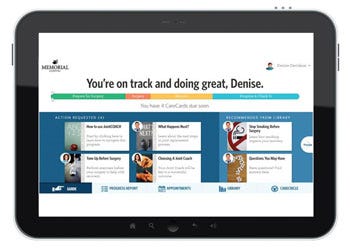
The JointCOACH platform offers patients information they'll need before, during, and after surgery. |
McCrone and McInerney emphasized that the Episode Performance Manager platform is scalable and will be able to expand as needed to meet any new bundled payment requirements.
The JointCOACH Platform
The other new tool, the JointCOACH platform, has been implemented in 30 hospitals so far. The tool enables patients to prepare before the operation with reminders about required tests and fasting, helps them understand what their procedure and hospital discharge process will be like, and gives them recovery and rehabilitation support. There are a number of videos on the platform, including rehabilitation exercises patients can perform. Patients also provide information about their home environment, a step that allows the hospital to determine the best postoperative recovery path for each person. "It's not realistic that no patient is going to go to a skilled nursing facility," McCrone pointed out.
McCrone described the tool as a good resource for hospitals to proactively stay connected with their joint replacement patients. Since CJR now shifts the responsibility for post-acute care costs squarely onto hospitals' shoulders, regular followup with patients is a must. Patients using JointCOACH are asked regularly how they are doing after the operation and care coordinators are alerted to any negative responses. That should allow hospitals to catch many potential complications early and hopefully reduce hospital readmissions. McCrone noted that JointCOACH doesn't require any additional work for physicians or hospital staff.
"You can triage the 10 patients that aren't answering the question positively or don't answer it at all, and give them a call to see what's going on to be more proactive to prevent that readmission," said McCrone.
Patients have been game to try JointCOACH so far, McCrone noted. "We're really excited about the engagement around [JointCOACH]. At the individual hospitals, we're seeing anywhere from 85-92% of patients feel prepared going through this program. Enrollment is about 70-90% into the program, depending on the hospital," he said, adding that SPS will try to get enrollment as close to 100% as possible.
As the program gains steam, SPS plans to evaluate potential ways to improve, such as whether patients are receiving the right content in the right way and whether the tool is driving lower costs for customers.
"We think it'll go far beyond our existing customer base . . . It's a need in the market. Hospitals are really trying to figure out how they're going to measure this risk," McCrone said.
Marie Thibault is the managing editor at MD+DI. Reach her at [email protected] and on Twitter @medtechmarie.
[Images courtesy of STRYKER]
About the Author(s)
You May Also Like