November 1, 2006
R&D DIGEST
|
Mark Prausnitz and Robyn Schlicher watch as ultrasonic pressure waves open cell membranes. |
Although drugs used in chemotherapy regimens can kill unhealthy cells, they can also harm healthy ones. Therapies that are able to target only the sick cells may help reduce side effects so that patients can enjoy better quality of life while being treated. New research shows that ultrasound may be a noninvasive way to send drugs directly into specific cells.
By increasing cell permeability, ultrasonic waves can target a specific cell, put holes in it, and deliver drug therapy. Researchers at Georgia Institute of Technology and Emory University (both in Atlanta) are using an ultrasound method that avoids healthy cells, thereby reducing the side effects of chemotherapy and other treatments.
This isn't quite the same ultrasound technique as that used for imaging a fetus or for shattering kidney stones. “We're somewhere in between,” says Mark Prausnitz, PhD, director of chemical and biomedical engineering at Georgia Tech. “You can leverage what is known about the medical device, but you need to make a different device that applies ultrasound in a special way that has reversible effects to drive drugs into [a cell].”
The researchers have assembled such a device using off-the-shelf components. A power supply provides sine waves that are amplified and fed to a piezoelectric transducer. The focused transducer directs acoustic energy to one location, which enables the device to target energy at high density in one spot and at lower density elsewhere.
|
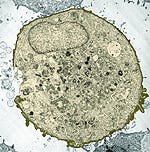
A scanning electron micrograph shows where ultrasound waves open the cell. |
Molecules enter the cells through holes created by the device. Ultrasonic pressure waves spontaneously form bubbles in the targeted area and make them oscillate. At low pressure, the bubbles get bigger, and at high pressure, they shrink. If driven hard enough, the bubbles collapse and create holes in cell membranes. These holes enable molecules as large as 50 nm in diameter to enter cells. The research found that the cell also repaired membranes themselves, closing the holes within minutes. Now the researchers need to determine how long the ultrasound waves should be applied.
Listening to the sounds could indicate when the ultrasound needs to be turned off. The bubbles make noise as they move around. Prausnitz has found a correlation between this noise and the effects on cells. When the bubbles are louder, more activity is occurring.
Although the team built a device for research purposes, it isn't developing a prototype of the makeshift technology. However, Prausnitz says, if approached by a device manufacturer, he'd be open to working with a company. “We're engineers, so it's important to make things that work. I'd very much like to see this technology ultimately become a product that helps people.”
Prausnitz envisions an integrated final device that has a practical interface between the ultrasonic transducer and the skin. Another useful component would be a “seek and treat” component that uses ultrasound to generate an image of a region. A labeling contrast method would identify the region, and then the user would be able to switch modes to apply therapy there.
For a better targeting effect, Prausnitz suggests performing the therapy in a minimally invasive, rather than noninvasive, manner. A catheter-based probe would be snaked up the appropriate vessel for a highly localized treatment.
Another, more-sophisticated option would be to coat the bubbles with a molecule that would preferentially bind to certain kinds of cells. This option would provide highly localized targeting on a cell-by-cell basis, says Prausnitz.
Although the concept of the device is promising, further studies must be conducted to assess how cells would respond when hit by ultrasound. It appears that a cell repairs itself after a hole is made, but it is unknown whether other changes are happening to the tissue.
Learning how to control the ultrasound exposure could also reduce the amount of stress put upon cells. Detailed studies will help the researchers understand the biochemical activities inside cells and shed light on whether these effects are detrimental.
The research was supported by the National Institutes of Health and the National Science Foundation. More details about the work are available in Ultrasound in Medicine and Biology 32, no. 6.
Copyright ©2006 Medical Device & Diagnostic Industry
About the Author(s)
You May Also Like