Originally Published MDDI May 2006 COVER STORY: ADHESIVESChanging adhesion options affects wound-care and transdermal applications. William Leventon
May 1, 2006
COVER STORY: ADHESIVES
|
Fast-cure silicones can be cured with a heat gun like the one shown here. |
They may be sticky, but adhesives that attach wound dressings and transdermal patches to the skin aren't stuck in the past. New developments abound, resulting in adhesives that are stronger, gentler, and longer wearing than older offerings.
But that's not all. These days, adhesives are more versatile than ever. “People want adhesives that hold things in place. But they also want some other functionality,” says George Cramer, vice president of marketing and commercial development for Adhesives Research Inc. (Glen Rock, PA). So Adhesives Research as well as many of its competitors are adding all sorts of capabilities to their products: breathability, conductivity, and drug delivery, to name a few. Adhesives can even help patients lose weight and wrinkles by playing a key role in a new type of product that could change the cosmetics industry.
Sticking with Wound Care
Not all adhesive advances involve changing formulations. Some are a matter of how adhesives are placed on substrates. In most cases, adhesives are applied in a continuous coating. But as its name suggests, the Macdots product from Mactac (Stow, OH) features adhesive applied in a noncontinuous dot formation.
Mactac can change the amount of adhesion provided by Macdots by changing the amount of adhesive coverage and the height of the dots on the substrate, notes Tim Mlnarik, the company's business development manager. “To make an adhesive layer less aggressive, you could use less adhesive. The dots could be smaller or there could be more distance between them,” he explains. Users might opt for a less-aggressive adhesive layer to minimize the trauma of removing bandages applied to chronic wounds.
Noncontinuous adhesive coatings also offer a higher moisture-vapor transmission rate (MVTR) than their continuous counterparts. A high MVTR facilitates the passage of exudates through the adhesive layer of bandages used to cover diabetic ulcers and other chronic wounds. “By selectively putting adhesive down in a dot formation, we build a natural conduit for moisture and vapor transmission,” Mlnarik says.
|
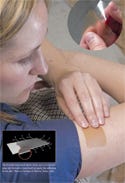
The transdermal patch shown here uses a noncontinuous dot formation (see inset) to apply the adhesive to the skin. Photos courtesy of Mactac (Stow, OH). |
Noncontinuous adhesive technology is also being developed by Adhesives Research, which takes a different approach than Mactac. Rather than a substrate covered with dots, the Adhesives Research version of noncontinuous adhesion consists of an adhesive layer riddled with pores. “If you looked at it through a magnifying glass, it would look like very fine Swiss cheese,” Cramer says. This porous adhesive allows moisture to pass through the adhesive layer, making it suitable for bandages used to soak up fluids from weepy wounds.
Besides allowing fluid passage, noncontinuous adhesives improve the breathability of wound dressings. Breathability was one of the main properties sought by Clozex Medical LLC (Wellesley, MA) in its search for an adhesive for its new wound-closure product. Called ClozeX, the device, which won a Medical Design Excellence Award in 2005, can close a wound without the use of sutures, staples, or glue. The ClozeX system includes strips of tape stuck to the skin on both sides of a wound. Interwoven straps attached to the tops of those tape strips hold the wound closed the way shoelaces hold a shoe closed.
Clozex wanted a breathable tape to be applied to the skin. During the company's search for the right adhesive, however, a number of suppliers offered products with thick adhesive layers that limited the breathability of the tape, which in turn caused maceration when applied to patients.
But Adhesives Research came up with a custom solution that satisfied Clozex. “The substrate itself breathes, and the application of the adhesive doesn't block off all the pores,” explains Ray Barbuto, vice president of manufacturing at Clozex. “It allows enough breathability so that elderly people and young children don't experience the maceration normally associated with an aggressive adhesive.”
In most cases, the ClozeX device stays in place for 5–15 days. So Clozex also needed an adhesive that would attach the tape strips to a patient's skin for the required time but not cause skin irritation.
Adhesive companies worldwide checked their commercial and experimental products to find something that would fill the bill. Most of the adhesives proposed for ClozeX caused severe skin irritation, Barbuto reports. But Adhesives Research came up with a skin-friendly acrylic-based adhesive that would stick to patients' skin for the required time. “We've had 100,000 units on people, and I think there have been two mild reactions to the adhesive,” he says.
Some acrylic-based adhesives made by Adhesives Research are hydrophilic. Applied to a wound dressing, adhesive layers made of hydrophilic acrylics can help manage moisture over a wet wound, Cramer says. This hydrophilicity distinguishes them from most acrylic adhesives, which can't absorb moisture and also maintain their integrity, he explains.
|
Adhesive layers of hydrophilic acrylics help control moisture in wound-care tapes. |
Hydrophilicity is a key attribute of hydrogels, which are essentially polymers swollen with water, according to Jerry Schalau, industry specialist at Dow Corning Corp. (Midland, MI). Wound dressings coated with hydrogel adhesives are very gentle when removed from the skin, Schalau says. The trade-off, he adds, is that they won't stay on the skin as long as some other adhesive options.
Although they offer a wet, almost gelatinous feel, hydrogels often require the presence of another adhesive to hold a wound dressing in place, Cramer notes. In the future, though, Cramer sees skin-friendly hydrogels that contain more-cohesive materials that will allow them to stand alone, without assistance from another adhesive. These hydrogel materials will have properties similar to those of conventional medical-grade tapes, he predicts.
Another type of hydrophilic material is the hydrocolloid. An adhesive with a very light tack, hydrocolloids come into direct contact with wounds, absorbing exudates and providing a moist environment that's conducive to healing, notes Katy Trudeau, global business leader at the TruMed facility of Brady Medical Converting (Burnsville, MN).
On the downside, Trudeau says, hydrocolloid becomes less absorbent as the material layer gets thinner. So bandages with hydrocolloid layers can be thick. “But if you have a blister bandage inside your shoe, you don't want it to have a 40-mil-thick hydrocolloid layer,” she says. “So now they're made a lot thinner. I think we can get the thickness down to 12 mil.”
Besides performing their traditional wound-care functions, some hydrocolloid adhesives are now impregnated with active ingredients that speed wound healing. For example, some fairly new hydrocolloid formulations include antimicrobial agents such as silver, Trudeau notes.
|
Bandages with hydrocolloid layers can now be made as thin as 12 mil and can include wound-healing agents. |
Transdermal Advances
Similarly, active ingredients are now being incorporated into adhesive coatings on transdermal patches. According to Cramer, it's a simpler design than old patch configurations that included drug reservoirs separate from the adhesives, whose sole function was to hold the patch in place. Simpler drug-in-adhesive systems can be easier to manufacture than old patch designs and may also allow a reduction in patch size, Cramer says.
Adhesives Research has developed adhesives for patches that deliver drugs through tissue inside the mouth. Drugs can be absorbed into the body through this tissue better than through the skin, according to Cramer. The challenge, he says, was to produce an adhesive that would stick to wet tissue inside the mouth, which is difficult to adhere to for any length of time.
Besides holding onto mouth tissue, the adhesive holds the drug to be delivered through that tissue. The drug is released as the erodable adhesive slowly dissolves in the mouth.
Another Adhesives Research product is designed for transdermal patches with an electrical drive. These patches include a tiny microprocessor, an electrical circuit, and two electrodes. Unlike so-called passive patches that rely on diffusion to pass drugs through the skin, these patches actively deliver their payloads at the press of a button on the patch, which triggers a charge that begins the drug-delivery process.
These patches feature two different polyisobutylene-based adhesives from Adhesives Research. One adhesive holds the patch in place and isolates the two electrodes from each other. The other adhesive is an electrically conductive material that helps connect the electrodes to the microprocessor.
Another promising group of adhesives designed for transdermal applications are rubber-acrylic hybrids. According to Cramer, a transdermal drug may be more soluble in a rubber than in an acrylic, so the rubber would serve as the drug reservoir. But that carries the risk of degrading the adhesive properties of the rubber. Hence the presence of the acrylic, which ensures that the patch adheres firmly to the skin.
Dual-Application Adhesives
A number of new adhesives are suitable for both wound-care and transdermal applications. NuSil Technology LLC (Carpinteria, CA) has introduced tacky silicone gels that can replace pressure-sensitive adhesives (PSAs) in wound-care applications. PSAs contain solvents that can cause skin irritation in some cases, says Mark Paulsen, NuSil's director for healthcare materials.
NuSil's tacky gels are very soft, compliant materials, which Paulsen compares to very sticky versions of gelatin. The gels “stick tenaciously to the skin,” Paulsen notes— perhaps even more tenaciously than PSAs. Nevertheless, he says, removing them from the skin may cause less trauma than the removal of PSA products. And like most silicones, he adds, the tacky gels are breathable, allowing the transmission of oxygen and moisture through a wound-care product.
Tacky gels are currently being evaluated for transdermal skin patches. According to Paulsen, silicones excel in drug-delivery applications because drugs are able to move freely through the silicone matrix. In addition, he notes, drugs can be released from the silicone matrix over a long period of time. “You can also tailor the gel to get the desired release rate for certain drugs,” he says.
NuSil is currently developing silicones with varying degrees of hydrophilicity. These polymers will be platforms for gels that can offer faster drug-release rates, Paulsen says. “A more-hydrophilic gel will allow a drug to move more readily through its matrix,” he explains. “So certain drugs will elute from a silicone gel matrix at faster rates if you can build a more-hydrophilic silicone.”
At Dow Corning, silicone gel adhesives are about to get a little more aggressive. According to Schalau, one of the downsides to the company's soft-skin adhesives (SSAs) is that they can't be used for long-term-wear applications. “It's a little counterintuitive that people would want higher adhesion in a product that's supposed to be gentle when you remove it,” he says. “But this is something we're working toward.”
Schalau expects his company's higher-adhesion SSAs to be on the market by next year. While traditional SSAs might provide up to six hours of wear time on a flat surface of the body, the new products might provide a full day of wear, he says. On a knuckle, he adds, traditional SSAs might last up to three hours, whereas the new products might provide 12–16 hours of wear time.
Because silicone adhesives are relatively expensive, Dow Corning is aiming its new SSAs at professional wound dressings used in places like hospitals, doctors' offices, and nursing homes. In hospitals, for example, the product could be used on dressings used to cover pressure ulcers. If such dressings were attached using Dow Corning's low-adhesion SSAs, Schalau says, they could shear off patients' bodies, leaving nothing to absorb wound exudates.
Although the new SSAs will adhere to the body approximately four times longer than their conventional counterparts, Schalau claims they'll still be relatively easy to remove. “It's not going to feel like water coming off of your skin when you take it off,” he says. “But it will still be considered gentle. We don't want people to say ‘ouch' when they take it off.”
Besides wound care, Schalau believes his company's higher-adhesion SSAs will be a good fit for applications involving transdermal drug delivery. “A traditional SSA might be adequate for a short-term therapeutic patch,” he says. “But it may not last long enough for most drug-delivery applications. Most of these therapies last at least 24 hours, so the patch has to remain on the skin at least a day. That's one of the drivers behind our new adhesive.”
Adhesion Trends
Thanks to new adhesives, both wound-care and transdermal products can adhere to the body for longer periods of time, despite activities like showering and exercising, according to Jennifer Ponti, director of sales and marketing for G&L Precision Die Cutting Inc. (San Jose). G&L is a converter that makes wound dressings and transdermal patches. Longer-wearing adhesives allow the use of longer time-release formulations on transdermal offerings, such as the 30-day birth-control products currently on the market, Ponti says.
Longer-lasting adhesives also reduce the number of bandage and patch changes, thereby improving patient comfort. “You don't have to keep trying to find a site on your body that hasn't been worn out because you have to peel tape off of it every day,” Ponti says. In hospitals, she notes, nurses no longer have to change a patient's dressing every day or several times a day. Instead, they can leave a dressing on a patient for a week or even a month, while monitoring the site to make sure there's no skin irritation in the area.
In addition to longer-wearing adhesives, Ponti and her G&L colleagues have noticed fine-tuning of specialized adhesives used in sensitive-skin applications such as elderly and neonatal care. “Manufacturers are formulating their adhesives so they're aggressive enough to stay on the skin. But when you peel them off of this very sensitive skin, there's very little damage done to the dermal layer,” she says.
To meet the need for gentler adhesives, Mactac has introduced a rubber-based product called ULA (ultralow adhesion), which allows painless removal of wound-care and transdermal products, according to Mlnarik. Most adhesive products become more difficult to remove the longer they're left on the skin, he says. But the ULA product doesn't keep building peel adhesion. Maximum adhesion is reached after about 30 minutes, he notes, resulting in painless removal—even when the adhesive is placed on hair. Nevertheless, he adds, a ULA-covered bandage will adhere firmly to the skin, even after being repositioned several times.
ULA isn't right for all wound-care and transdermal applications. Its limited breathability makes it unsuitable for wound-care applications lasting longer than 24 hours. In addition, its peel adhesion limit isn't always an advantage. In some cases, Mlnarik notes, it's desirable for adhesion to continue building after 30 minutes. Such cases include situations in which a bandage is subjected to high shear loads or other stresses.
Mlnarik forecasts strong demand for firmly adhering but easy-to-remove adhesives like ULA for use on products such as antiwrinkle and weight-loss patches. For years, Trudeau says, OEMs have been developing such patches, which include adhesives loaded with active ingredients for all sorts of cosmetics applications.
Trudeau's company is currently working with OEM customers on a number of transdermal patches for the cosmetics industry. These projects and many others like them will eventually result in “an explosion of cosmetic transdermal patches on the market,” she predicts.
“There's been a lot of chatter in the industry about when these things will be coming out,” Trudeau reports. Her guess: a year or two at the most. In any case, she says, “It's only a matter of time.”
William Leventon is a freelance writer based in Somers Point, NJ.
Copyright ©2006 Medical Device & Diagnostic Industry
About the Author(s)
You May Also Like