thumbnail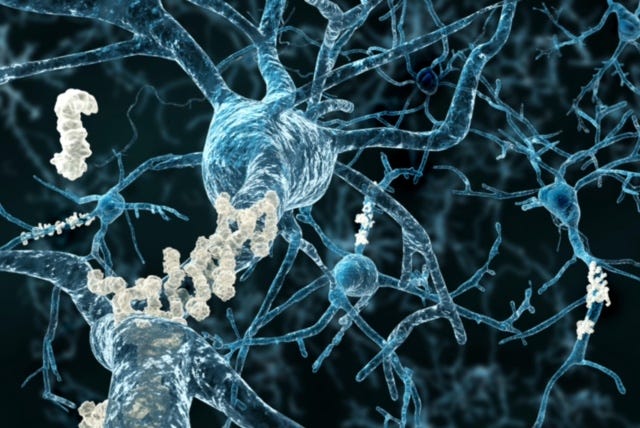
IVD
Roche Lands Breakthrough Designation for Alzheimer’s TestRoche Developing a Blood Test for Alzheimer's Disease
The Basel, Switzerland-based company’s test looks for the presence of amyloid pathology in patients suspected of having Alzheimer’s.
Sign up for the QMED & MD+DI Daily newsletter.


.png?width=700&auto=webp&quality=80&disable=upscale)
.png?width=700&auto=webp&quality=80&disable=upscale)




























.png?width=300&auto=webp&quality=80&disable=upscale)