How can drug delivery advance beyond the traditional vial and syringe?
The pharmaceutical industry has followed a path that clings to traditional medicine as it simultaneously pursues innovation. Perhaps no area of the business illustrates this as clearly as that of parenteral administration of therapeutics. What is the status of legacy versus disruptive drug-delivery methods? Where should we be focusing our attention as we serve the pharma client seeking guidance on parenteral technologies, pitfalls, and profitability?
As a company focused on custom packaging design, we see our customers struggle with this every day—traditional methods ensure a quick go-to market strategy, while innovative delivery methods take longer (but could be a clear point of differentiation in a crowded market). We often see new drug therapies enter the market with traditional packaging and delivery methods; then, as the medicine gains traction and popularity, the delivery method is often reviewed and even redesigned.
The Traditional “Shot,” Tried and True
As we know, traditional injections rely on syringes and hypodermic needles filled from ampoules and vials. The overall design, materials, and delivery of hypodermic injections have remained largely unchanged for more than 70 years. And even as new delivery technologies have emerged, the vial and ampule markets continue to show strong forecasts. Current forecasts predict steady growth through at least 2028.
Several factors contribute to the enduring demand. Low cost, universal use, and proven reliability generally make the hypodermic injection the fastest way for medicines to reach market in the process of conducting clinical trials. Once a formula has been successfully established and marketed, moving on to prefilled syringes is a shift that can be explored.
The Prefilled Syringe
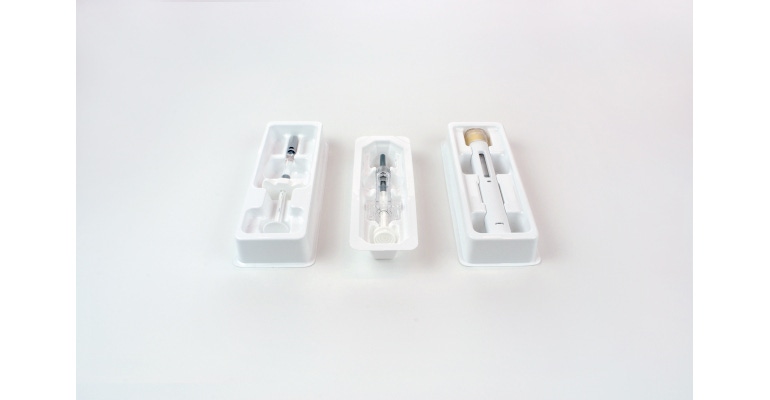
The popularity and still-rising demand for the prefilled syringe (PFS) make it hard to believe that it has been on the market for more than 40 years. Who remembers the first PFS hitting the market as a breakthrough heparin delivery method? Many of us still feel like the PFS is relatively new! The advantages of a delivery system that serves as both the packaging and the administration are easily recognized. There are two basic PFS types: those with and without a cartridge. Prefilled syringes with cartridges are often used in vaccine delivery, while staked-in (integrated needle as part of the syringe) serve emergency needs. Prefilled syringes without an integrated needle require the attachment of a needle. The newest design option is the dual-chamber PFS that allows two drugs to be co-delivered or pairs a lyophilized drug with a diluent. The convenience, rapid administration, accuracy, drug waste reduction, and enhanced patient safety offered by the various forms of PFS are often preferred in both clinical and patient-managed care settings.
And if the PFS is not really “new” anymore, then what drives the rapidly expanding demand? Certainly, continued advancements in design versatility and increasing numbers of biologics suited to the PFS are factors. Additionally, emerging high-tech materials (i.e., polymers that don’t interact with contents) continue to mitigate some PFS challenges (i.e., stability, siliconization, tungsten residues, glass stress). It is reasonable to conclude that current limitations will continue to be eclipsed by innovation.
Auto-Injectors
The discussion of prefilled syringes naturally leads to the next parenteral route, the auto-injector. The auto-injector was originally developed in the 1970s to deliver nerve gas antidote for the U.S. military. Developer Sheldon Kaplan also created the mainstream version to deliver epinephrine for anaphylaxis, with the famed EpiPen receiving FDA approval in 1987. The pens are fast, easy for anyone to use with no training, and can effect life-saving outcomes. Patients and caregivers report ease of use and significantly reduced administration discomfort, further galvanizing the interest of pharmaceutical clients in new opportunities for auto-injection delivery devices. Human factor testing in at least one study supports that while many patients will be successful in self-administering injections from a PFS, patients given auto-injector devices demonstrated total success, even without additional training for the device.
Auto injectors (both disposable and re-usable, with the former capturing the largest share) are also gaining ground in a wider range of treatment areas, including MS, RA, diabetes, and heart disease. Auto injectors are predicted to reach 104.9 billion by 2025 (CAGR 17.9%). Increasing instances of anaphylaxis, generic availability, upcoming expiry of biologics patents, and more targeted medicines all play a role in the future of auto injectors.
Intranasal Delivery
And finally, the newest delivery method that has taken the stage during the last decade has been intranasal drug delivery. There is a lot of potential. Absorption takes place through nasal lymphoid tissue. Highly vascularized and easily accessible, intranasal delivery offers high bioavailability, rapid absorption, and avoidance of first-pass effect common with gastrointestinal administration. There is also the potential compliance advantage of low patient resistance to intranasal delivery. Nasal drops and sprays are already familiar and perceived as painless and well-tolerated, adding to the appeal of further R&D for this method. As with all parenteral drug-delivery routes, intranasal is not without challenges and limitations. Dosing, for example, is limited as the absorption area is small compared with that of other routes. Additionally, only certain drug types are currently suited to intranasal delivery for a variety of reasons. It is a topic to watch—and investigate—as we go forward.
In conclusion, and in our opinion, it is possible that demand for original syringe, hypodermic needle, and drug transfers from vials and ampoules could finally see declining demand in the not-so-distant future, but they will likely always have a purpose and place. There are advantages to starting with a tried-and-true solution and progressing to a more-innovative drug-delivery method down the line. Speed, security, and patient familiarity are all advantages to starting with the more-traditional solution. Packaging takes on a more important role as therapies transition from vials to patient-administered delivery systems. Gaining market knowledge and time allow for clients to refine and innovate in their next round of packaging. Other parenteral drug-delivery routes, including those less studied and not widely implemented to date, hold exciting potential for pharma clients and patients. There is no limit to the refinements and possibilities that could transform how medicines are introduced into and function within the human body in the months and years ahead.
About the Author(s)
You May Also Like




